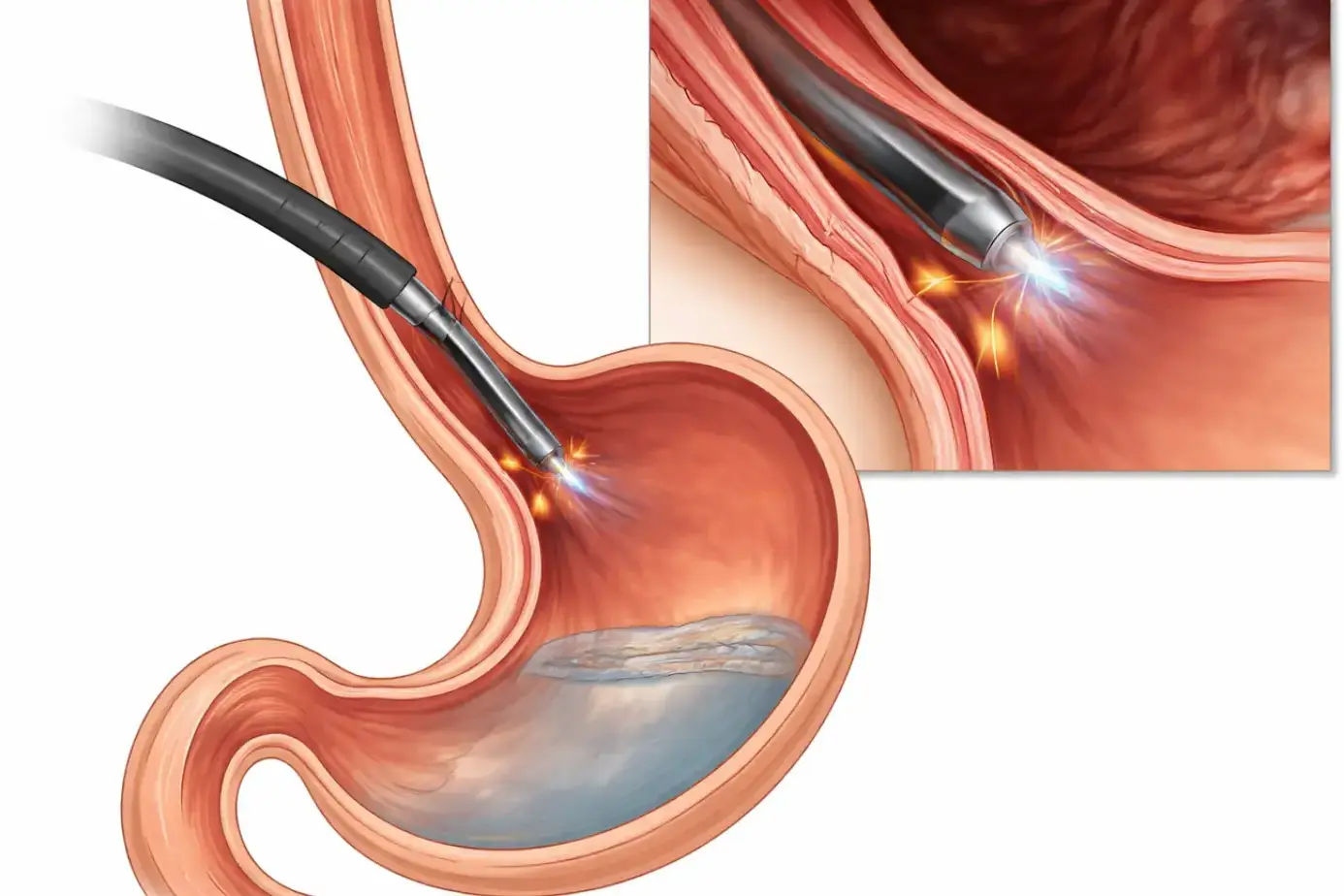
Did you know that duodenal ulcers affect approximately 10% of the global population?
Table of Contents
ToggleIf you’ve ever experienced persistent stomach pain or discomfort, it could be a sign of a duodenal ulcer. This common condition, also known as a peptic ulcer, develops in the lining of the duodenum, the first part of the small intestine. Duodenal ulcers can cause a range of symptoms, from mild discomfort to severe pain that disrupts your daily life.
In this article, we will dive deeper into the world of duodenal ulcers. You will discover the symptoms, causes, diagnosis, and treatment options available for this condition. Understanding the ins and outs of duodenal ulcers is crucial for effectively managing your stomach health and improving your overall well-being.
Understanding Duodenal Ulcer Symptoms
If you suspect you may have a duodenal ulcer, it is crucial to be aware of the common symptoms associated with this condition. By recognizing these symptoms, you can take appropriate actions and seek medical attention to address the issue effectively.
One of the primary symptoms of a duodenal ulcer is abdominal pain. This pain is often described as a burning or gnawing sensation that occurs in the upper abdomen, between the belly button and breastbone. The pain may come and go, but it is typically more intense when the stomach is empty, such as between meals or during the night.
Another prominent symptom is nausea. People with duodenal ulcers often experience a feeling of queasiness or an urge to vomit. This symptom may be accompanied by vomiting, which can provide temporary relief but does not address the underlying issue.
Bloating is also a common symptom of duodenal ulcers. It is characterized by a feeling of fullness or tightness in the abdomen, even after consuming small amounts of food. This discomfort is caused by the excessive production of stomach acid that irritates the delicate lining of the duodenum.
Heartburn and acid reflux are additional symptoms that may indicate the presence of a duodenal ulcer. These occur when stomach acid flows back into the esophagus, causing a burning sensation in the chest or throat.
In some cases, duodenal ulcers can lead to weight loss or poor appetite. The persistent pain and discomfort can affect eating habits, leading to a decrease in food intake and subsequent weight loss.
Although less common, duodenal ulcers can cause bloody or dark stools. This occurs when the ulcer bleeds, and the blood mixes with the stool, resulting in noticeable color changes.
Remember that individual experiences may vary, and not everyone may exhibit the same combination or severity of symptoms. If you are experiencing any of these symptoms or suspect you may have a duodenal ulcer, it is advisable to consult a healthcare professional for a proper diagnosis and appropriate treatment.
Causes of Duodenal Ulcers
Duodenal ulcers can have multiple causes, and understanding these factors is crucial for preventing and managing this condition. By making informed choices, you can reduce the risk of developing duodenal ulcers and promote a healthy digestive system.
H. pylori Infection
One of the primary causes of duodenal ulcers is infection with H. pylori bacteria. These bacteria can weaken the protective layer of the stomach and duodenum, leaving them susceptible to damage from stomach acids.
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs)
Regular use of NSAIDs, such as aspirin and ibuprofen, can irritate the stomach lining and contribute to the formation of duodenal ulcers. These medications reduce inflammation but can also increase the risk of ulcers when taken for an extended period or in high doses.
Excessive Stomach Acid Production
Individuals who produce excessive stomach acid may be more prone to duodenal ulcers. The increased acid levels can erode the protective lining of the duodenum and lead to ulcer formation.
Smoking
Smoking has been linked to an increased risk of duodenal ulcers. The chemicals in cigarettes can weaken the protective barrier in the digestive system, making it more vulnerable to ulcers.
Stress and Lifestyle Factors
While stress itself may not directly cause duodenal ulcers, it can worsen symptoms and delay the healing process. Additionally, certain lifestyle factors such as alcohol consumption and a diet high in spicy or fatty foods can increase the risk of developing ulcers.
By addressing these potential causes and adopting healthier habits, you can minimize the risk of developing duodenal ulcers and maintain optimal digestive health.
Diagnosing a Duodenal Ulcer
In order to identify and confirm the presence of a duodenal ulcer, healthcare professionals utilize various diagnostic procedures and tests. These medical examinations play a crucial role in determining the appropriate treatment plan for patients.
When you visit a healthcare provider to diagnose a duodenal ulcer, they will typically begin by conducting a comprehensive medical history interview, asking you questions about your symptoms, medical background, and lifestyle habits. This initial assessment helps them gain a holistic understanding of your condition.
One common diagnostic test for duodenal ulcers is an upper gastrointestinal (GI) endoscopy. This procedure involves using a flexible tube with a light and camera attached, known as an endoscope, to examine the esophagus, stomach, and duodenum. Through this test, healthcare professionals can visualize any ulcers or other abnormalities in the digestive tract.
Additionally, your healthcare provider may recommend a barium swallow or barium meal. These tests involve consuming a liquid containing barium, a contrast material that helps highlight the structures of the upper digestive system in X-rays. By examining the X-ray images, healthcare professionals can identify potential ulcers or other abnormalities.
In some cases, laboratory tests may be conducted. A stool test can be used to detect the presence of a bacterium called Helicobacter pylori, which is a common cause of duodenal ulcers. Additionally, a blood test may be performed to check for the presence of antibodies that indicate a previous infection with H. pylori.
Once a duodenal ulcer is diagnosed, it is crucial to discuss the results with your healthcare provider and establish an appropriate treatment plan based on your individual circumstances.
Summary of Diagnostic Procedures for Duodenal Ulcers
Below is a summary of the diagnostic procedures used to diagnose duodenal ulcers:
| Diagnostic Procedure | Description |
|---|---|
| Upper Gastrointestinal (GI) Endoscopy | An endoscope is used to visualize the esophagus, stomach, and duodenum for ulcers or abnormalities. |
| Barium Swallow/Barium Meal | A contrast material is consumed, and X-rays are taken to detect ulcers or abnormalities. |
| Stool Test | A test to detect the presence of Helicobacter pylori, a common cause of duodenal ulcers. |
| Blood Test | A test to check for antibodies indicating a previous H. pylori infection. |
Treatment Options for Duodenal Ulcers
If you have been diagnosed with duodenal ulcers, there are several treatment options available to help you manage this condition and promote healing. The choice of treatment depends on the severity of your symptoms, the underlying cause of the ulcers, and your overall health. In most cases, a combination of medical intervention and lifestyle changes is recommended for optimal results.
Medical Treatment
Medication plays a crucial role in treating duodenal ulcers by reducing stomach acid production and promoting healing of the damaged tissues. Your healthcare provider may prescribe the following medications:
- Proton Pump Inhibitors (PPIs): These drugs are highly effective in reducing stomach acid production and providing relief from ulcer symptoms. PPIs such as omeprazole, pantoprazole, and esomeprazole are usually taken once a day.
- H2 Receptor Blockers: These medications also reduce stomach acid production but are not as potent as PPIs. They can be used as an alternative to PPIs or in combination with them.
- Antibiotics: If your duodenal ulcers are caused by an infection with the bacteria Helicobacter pylori, your doctor may prescribe a course of antibiotics, such as amoxicillin and clarithromycin, to eradicate the bacteria.
It is important to take your medications as prescribed and complete the full course of treatment to ensure effective eradication of the ulcers and enhance the healing process.
Lifestyle Changes
In addition to medication, making certain lifestyle changes can help manage duodenal ulcers and prevent their recurrence. Here are some key lifestyle interventions:
- Dietary Modifications: Avoid foods and beverages that can irritate the stomach lining, including spicy foods, caffeine, alcohol, and acidic foods. Opt for a nutritious diet rich in fruits, vegetables, whole grains, and lean proteins.
- Stress Management: Stress can exacerbate ulcer symptoms. Incorporate stress-reducing activities into your daily routine, such as exercise, meditation, yoga, or deep breathing exercises.
- Smoking Cessation: Smoking can delay the healing process and increase the risk of ulcer recurrence. Quitting smoking is essential for better ulcer management and overall health.
- Limit Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): NSAIDs, including aspirin and ibuprofen, can irritate the stomach lining and worsen ulcer symptoms. Talk to your healthcare provider about alternative pain relief options if necessary.
By implementing these lifestyle changes, you can support the healing process and reduce the risk of future ulcer flare-ups.
To find out the most suitable treatment options for your specific condition, consult with a healthcare professional. They will assess your individual circumstances and develop a personalized treatment plan to effectively manage your duodenal ulcers.
Preventing Duodenal Ulcers
Preventing duodenal ulcers is crucial for maintaining a healthy digestive system and avoiding the discomfort and pain associated with this condition. By implementing effective strategies and making simple lifestyle changes, you can significantly reduce the risk of developing duodenal ulcers or experiencing a recurrence.
Eat a Balanced and Nutritious Diet
Avoiding certain foods and incorporating others into your diet can help prevent duodenal ulcers. Limit your intake of spicy and fatty foods, as they can irritate the stomach lining. Instead, opt for a diet rich in fruits, vegetables, whole grains, and lean proteins. These foods provide essential nutrients and promote good digestive health.
Manage Stress Levels
Chronic stress can increase the production of stomach acid, which can contribute to the development of duodenal ulcers. Engaging in stress-management techniques such as meditation, deep breathing exercises, and regular physical activity can help reduce stress levels and support a healthy digestive system.
Avoid Smoking and Excessive Alcohol Consumption
Smoking and excessive alcohol consumption are known risk factors for duodenal ulcers. These substances can irritate the stomach lining and increase acid production. By quitting smoking and limiting alcohol intake, you can lower your risk of developing ulcers and promote overall gastrointestinal wellness.
Practice Good Hygiene
Proper hygiene, especially handwashing, is essential for preventing infections that can lead to duodenal ulcers. Avoiding close contact with individuals who have infections, particularly those caused by the Helicobacter pylori bacteria, can significantly reduce your risk.
Take Nonsteroidal Anti-inflammatory Drugs (NSAIDs) with Caution
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and aspirin can increase the risk of duodenal ulcers. If you need to take these medications, always follow the recommended dosage and duration. Consult with your healthcare provider about alternative pain management options if you are prone to ulcers.
| Prevention Strategies | Key Benefits |
|---|---|
| Eating a balanced and nutritious diet | Provides essential nutrients for good digestive health |
| Managing stress levels | Reduces acid production and supports a healthy digestive system |
| Avoiding smoking and excessive alcohol consumption | Reduces irritation to the stomach lining and lowers the risk of ulcers |
| Practicing good hygiene | Prevents infections that can lead to duodenal ulcers |
| Taking NSAIDs with caution | Reduces the risk of ulcers associated with these medications |
Conclusion
In conclusion, duodenal ulcers are a common stomach condition that can cause discomfort and pain. By being aware of its symptoms, causes, and treatment options, you can take proactive steps to manage and improve your overall digestive health.
If you suspect you have a duodenal ulcer, it is important to consult with a healthcare professional for a proper diagnosis and personalized treatment plan. They can guide you in the right direction and recommend the most suitable approach based on your individual needs.
Remember, prevention is always better than cure. By adopting a healthy lifestyle, including a balanced diet and regular exercise, you can reduce your risk of developing duodenal ulcers. Additionally, managing stress levels and avoiding risk factors such as smoking and excessive alcohol consumption can also contribute to maintaining a healthy digestive system.
FAQ
What is a duodenal ulcer?
A duodenal ulcer is a stomach condition characterized by the formation of open sores on the lining of the duodenum, the first part of the small intestine.
What are the symptoms of a duodenal ulcer?
Common symptoms of a duodenal ulcer include abdominal pain, burning or gnawing sensation in the stomach, indigestion, nausea, vomiting, and unintentional weight loss.
What causes duodenal ulcers?
Duodenal ulcers are primarily caused by a bacterial infection called Helicobacter pylori (H. pylori) and long-term use of nonsteroidal anti-inflammatory drugs (NSAIDs). Other factors such as smoking, excessive alcohol consumption, and stress can also contribute to the development of duodenal ulcers.
How are duodenal ulcers diagnosed?
Healthcare professionals diagnose duodenal ulcers through a combination of medical history review, physical examination, and tests such as upper endoscopy, X-ray, or breath tests to detect H. pylori infection.
What are the treatment options for duodenal ulcers?
Treatment options for duodenal ulcers may include medications to reduce stomach acid production, antibiotics to eradicate H. pylori infection, and lifestyle changes such as avoiding NSAIDs, managing stress, and adopting a healthy diet.
How can duodenal ulcers be prevented?
Duodenal ulcers can be prevented by maintaining good hygiene, avoiding prolonged use of NSAIDs, managing stress, quitting smoking, limiting alcohol consumption, and following a balanced diet with enough fiber and probiotics.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.