Rectal prolapse happens when the rectum comes out through the anus. This makes the rectum turn inside out. It can cause both physical discomfort and emotional stress.
Table of Contents
ToggleThis problem affects a small part of the population, roughly 0.5%. It’s more common in women, especially those over 50. Although we’re not sure what exactly causes it, things like chronic constipation, giving birth, getting older, and family history are thought to be factors.
Introduction to Rectal Prolapse
Rectal prolapse is a condition where the rectum, the lowest part of the large intestine, falls out of the body through the anus. This can either happen slowly or all of a sudden. While it’s uncomfortable and can be embarrassing, it’s not often an emergency. But, it’s crucial to get medical help to stop it from getting worse and find the right treatment.
This issue mainly affects women and those over 50. Surprisingly, one-third of those with rectal prolapse have never given birth. If someone deals with chronic constipation and pushes too hard when they go to the bathroom, their chances of getting rectal prolapse go up.
[Rectal prolapse overview] can lead to problems like not being able to control bowel movements. This affects a huge number of people with the condition. But, there are many ways to treat it, including a successful surgery called rectopexy. This surgery is 97% effective at fixing the problem for the long term. However, very rarely, this surgery might harm a nerve linked to men’s sexual health.
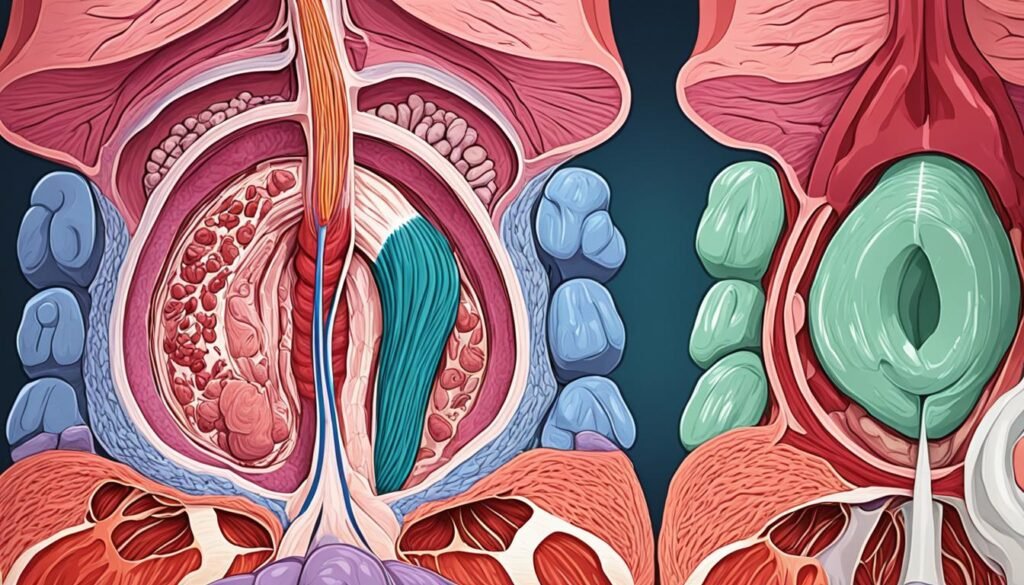
what is rectal prolapse
Definition of Rectal Prolapse
Rectal prolapse means the rectum, at the end of the large intestine, slips out the anus. It happens when the rectum’s regular inside attachments are lost. Then, it can push out through the anus. You might see a fleshy, red mass outside the body. This is the protruded rectum.
Prevalence and Risk Factors
About 0.5% of the population deals with rectal prolapse. It’s seen more in women over 50. The cause isn’t fully known. Yet, common factors include constant constipation, giving birth, getting older, and family history.
In men, this issue might occur at a younger age, less than 40. They might have defecation issues, autism, delays in development, or mental health concerns. These men could be on several medications.
Causes of Rectal Prolapse
Rectal prolapse has many causes. It’s important to know them to treat the condition well. The primary reasons for prolapse are chronic constipation, hard straining, giving birth, getting older, and genetic factors.
Chronic Constipation and Straining
Chronic constipation, straining during bowel movements, is a main cause of rectal prolapse. When a person strains a lot, the muscles and tissues that hold the rectum weaken. This can make the rectum slowly push out through the anus. About 30-67% of those with rectal prolapse have had chronic constipation.
Childbirth and Aging
Once, people thought that having several vaginal births greatly increased the risk of rectal prolapse. We now know this isn’t always true since up to 35% of those with prolapse have never given birth. Getting older also plays a big role, especially in women over 50. As we age, our pelvic floor muscles and tissues can become weaker, making prolapse more likely.
Genetic Predisposition
There might be a genetic link to rectal prolapse. Some people seem more likely to get it because of family traits. We don’t fully understand which genes are involved. But, experts think that certain people have pelvic floor muscles and tissues that are naturally weaker.
Symptoms of Rectal Prolapse
The main sign of rectal prolapse is when the rectum bulges out through the anus. At first, this might only happen after going to the bathroom. But as it gets worse, the rectum can stick out more and maybe even stay out. Sometimes, it needs to be put back in place manually.
Protrusion from the Anus
A fleshy, red mass that comes out of the anus is a clear sign of rectal prolapse. This part that sticks out can cause discomfort and be very embarrassing for those it happens to.
Bowel Dysfunction
Rectal prolapse can cause bowel problems. For example, about half of the people with this issue suffer from constipation. The prolapsed rectum can block the normal flow of stool. Weak anal muscles can also lead to fecal incontinence, causing the person to lose control of their bowel movements.
Bleeding and Mucus Discharge
A prolapsed rectum can get sore and start bleeding. This often leads to mucus coming from the anus as well. Both these symptoms are uncomfortable and can make the person feel embarrassed.

Differentiating Rectal Prolapse from Hemorrhoids
Rectal prolapse and hemorrhoids both involve tissue coming out of the anus. But, they are different. Hemorrhoids are swollen blood vessels. Rectal prolapse is when the rectum comes out of the anus. It’s vital to know the difference. This helps in choosing the right treatment.
Hemorrhoids lead to pain in the anal area, blood in the stool, and itching. They also cause swelling and hard lumps. On the other hand, rectal prolapse signs include constipation and rectal pain. You might see a bulge after coughing or lifting. There could also be mucous in the stool, or trouble controlling bowel movements. For doctors to tell the two apart, they look at how the problem looks and feels.
Doctors might use video-proctoscope or MRI Dynamic defecography to find out if it’s rectal prolapse. Understanding the symptoms of each, and getting the right diagnosis, is crucial. This is key to treat rectal prolapse and hemorrhoids correctly. It helps in reducing the pain and discomfort.
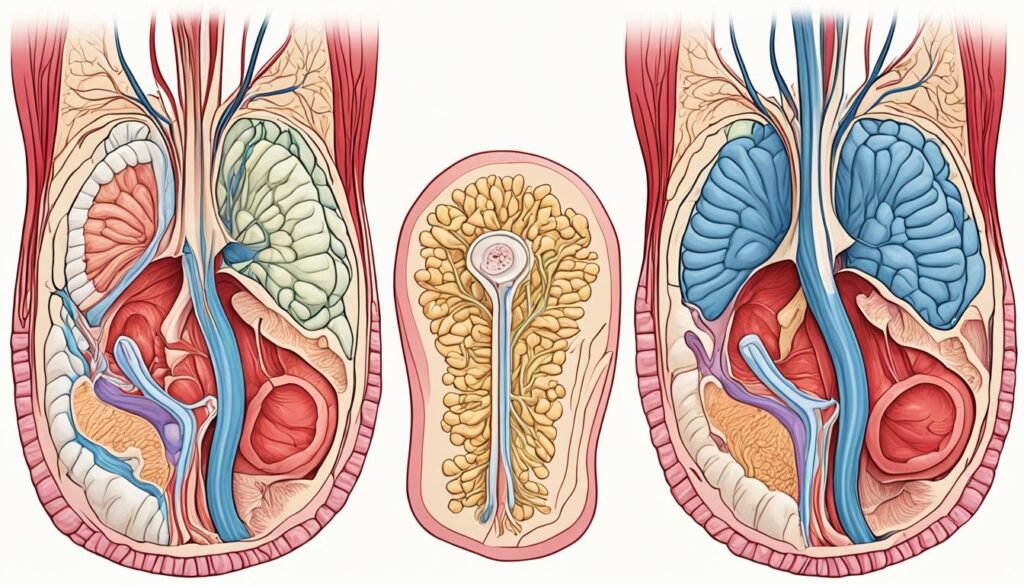
Diagnosis of Rectal Prolapse
Diagnosing rectal prolapse accurately is key for a good treatment. A colon and rectal surgeon will start with a detailed physical check. They will look at how far the prolapse has occurred.
Physical Examination
Your doctor will check you and ask to push like when you go to the bathroom. This checks the prolapse’s severity. They might also want photos of the prolapse when you’re at home.
Diagnostic Tests
If the physical check isn’t clear, more tests might be needed. These will help confirm rectal prolapse and rule out other issues. Tests like defecography, anorectal manometry, colonic transit study, and colonoscopy could be done.
These tests, along with a detailed physical exam for rectal prolapse, give the doctor a full picture. Then, they can design a treatment just for you.

Treatment Options for Rectal Prolapse
Dealing with rectal prolapse offers both non-surgical and surgical choices. It’s key to weigh the benefits and drawbacks with your doctor. This helps figure out the best route for your case.
Non-Surgical Treatments
In the early stages, doctors look at non-surgical options first. These methods might involve using medications to soften stools and reduce the need to strain. They could also suggest trying to push the rectum back on your own. But these routes often aren’t permanent fixes. So, surgery might be the real solution.
Surgical Treatments
For cases that are quite severe or keep coming back, surgery is the usual path. The exact surgical method will be decided based on how bad the prolapse is, your health, and what your doctor prefers. There are types of surgery done through the abdomen or the perineum.
Abdominal Approaches
In abdominal rectopexy, doctors move the rectum from its surroundings and fasten it to the sacrum. This technique is mostly very successful. Only a small number of patients see the prolapse happening again. Sometimes, part of the colon is taken out to make the bowels work better.
Perineal Approaches
Perineal surgery like the Altemeier or Delorme methods are chosen for some patients. This is mainly for older or less healthy people not fit for abdominal surgery. The surgery is focused on the area around the anus and genitals. It takes out the part that has prolapsed and fixes the rest in place. Though this way is more likely to see the prolapse return, it might be the better pick for a few.
Complications and Risks
If left untreated, rectal prolapse can cause severe issues. This includes the prolapse getting worse, and permanent fecal incontinence. This happens because the anal sphincter muscles can stretch and get damaged. ”
In rare cases, the prolapsed tissue can get incarcerated or strangulated. This turns into a medical emergency. Surgery for rectal prolapse also has its own risks. These include possible bleeding, infection, and issues with sexual function. There’s also a small chance that the prolapse might come back after surgery.
Women are at a higher risk for rectal prolapse. About 80 to 90% of adults with this issue are female. The risk increases with age, especially for those over 50. Complications may cause rectal bleeding. They might also damage the sphincter muscles and nerves. This can lead to or make bowel control problems worse.”
Statistics say rectal prolapse is more common in women and older people. These complications can cause rectal bleeding and worsen bowel control.
It’s crucial to get medical help for rectal prolapse. Leaving it untreated can lead to major problems. For adults, surgery is often recommended. For children, the focus is on treating things like constipation or diarrhea.”
Taking action early can prevent serious complications. So, seeing a doctor is important for the best outcome.”
Recovery and Lifestyle Modifications
After getting treated for rectal prolapse, you might stay in the hospital for just a night. You’ll start with liquids, moving on to solid foods. Your doctor will watch your bowel activity. They’ll make sure it’s getting back to normal smoothly. They’ll tell you to eat more fiber, drink lots of water, work out often, and keep a good weight. You may also take medicines to make bowel movements easier for a while.
It’s important to change your life a bit to avoid rectal prolapse happening again. This means:
- More fiber from fruits, veggies, and whole grains makes your stool soft. This means less pressure when you go.
- Drink enough water to keep your bowel work in check.
- Working out helps your body in many ways, like making your bowels work better.
- Keeping a healthy weight stops too much pressure on your pelvic area.
- Avoiding big lifts and hard pushes when you go to the bathroom. This helps you steer clear of rectal prolapse.
These lifestyle changes for rectal prolapse really make a difference. They can stop new episodes and boost how good you feel every day.
Rectal Prolapse in Children
[Rectal prolapse in children] is less common than in adults, but it does happen in some kids. Those with chronic health issues like constipation, poor nutrition, and certain diseases might be more at risk.
Often, a child’s pediatrician can treat [rectal prolapse]. They focus on the root cause, which might be constipation or a chronic health issue. If it’s more severe or keeps happening, the child might see a specialist for help.
In kids, the most cases of [rectal prolapse] occur before they turn one. Those who get it after age four might have an ongoing health issue making them more likely to have a prolapse. It affects boys and girls equally, mostly between age one and three.
Constipation is closely linked to [rectal prolapse] in American kids. Luckily, about 90% of those who develop it before age three can be helped without surgery. Kids with cystic fibrosis need special care to prevent this problem.
When caught early, [rectal prolapse] between 9 months and 3 years can be managed well. It shouldn’t lead to further health issues. A team of doctors working together ensures the best care for these children.
Preventing Rectal Prolapse
Keeping a healthy lifestyle is key to avoid or deal with rectal prolapse. Yes, adjusting your diet and lifestyle can work wonders. This way, you lessen the chances of getting this condition or make the symptoms better.
Dietary Changes
Focusing on what you eat can go a long way. You should eat more fiber found in fruits, veggies, and whole grains. This makes your stool softer, meaning you won’t have to strain as much when you go to the bathroom. And, drink plenty of water to help keep things moving smoothly.
Lifestyle Adjustments
Changing how you live can also keep rectal prolapse at bay. Do exercise to make your pelvic floor muscles stronger. This can help a lot. Also, being at a healthy weight is crucial. It prevents your pelvis from bearing too much pressure.
Avoid heavy lifting and don’t push too hard when you’re on the toilet. These things can reduce the risk of rectal prolapse.
Impact on Quality of Life
Rectal prolapse can change your life for the worse. It brings physical pain, self-consciousness, and problems with normal body functions. These difficulties might make you pull back from social life, feel worried, or get very sad. They can also mess up your day-to-day life and close relationships.
But the good news is, you can get help. By seeing a doctor and getting the right treatment, things can get better. You can start feeling like yourself again and enjoy life more.
Research shows rectal prolapse is not very common, happening to about 2.5 out of 1,000 people. It’s seen more in people born female. The risk goes up if you’re over 50. Kids can get it too, if they have health issues like ongoing diarrhea. This can also happen to older people with a history of constipation or issues with their pelvic floor.
If you have a rectal prolapse, getting help is important. Without care, it can cause serious damage. But with the right treatment, you can get back to a better life.
Conclusion
Rectal prolapse can greatly impact life quality. It brings discomfort, embarrassment, and affects daily life. While the exact cause is unknown, factors like chronic constipation and aging are thought to be key. Getting diagnosed early is crucial.
There are different ways to treat rectal prolapse. Some choose non-surgical methods. These include changing your diet and how you live. Others may opt for surgery. This depends on the severity of the condition and your health. But with the right treatment, you can improve your well-being.
If you have rectal prolapse symptoms, see a doctor. They will find out what’s wrong and suggest ways to help you. With timely treatment, you can manage rectal prolapse. This will let you feel better and more confident again.
FAQ
What is rectal prolapse?
Rectal prolapse is when the rectum turns inside out. The rectum, part of the large intestine, pushes out through the anus.
This happens when its normal attachments loosen.
What are the symptoms of rectal prolapse?
Primary signs include the rectum bulging out of the anus. Other symptoms are constipation, leakage, and blood/mucus in the stool.
These signs may also cause discomfort.
What causes rectal prolapse?
Doctors are not certain about its origin. However, some known factors are long-term constipation, childbirth, getting older, and family history.
How is rectal prolapse diagnosed?
Diagnosing it often starts with a physical check-up. The doctor might also suggest defecography, anorectal manometry, or a colonoscopy.
These tests help confirm the problem and rule out other health issues.
What are the treatment options for rectal prolapse?
There are non-surgical and surgical treatments. Non-surgical methods involve using stool softeners or gently pushing the rectum back in place.
Surgery options include rectopexy, Altemeier, or Delorme procedures.
What are the risks and complications of rectal prolapse?
Without treatment, it can lead to serious issues like worsening prolapse or permanent leakage. Surgery risks include infection and the possibility of the issue coming back.
How can rectal prolapse be prevented?
People can reduce the risk by eating more fiber and drinking plenty of water. Staying physically active and managing body weight help too.
It’s vital to treat chronic constipation to prevent rectal prolapse.
Can rectal prolapse occur in children?
Yes, but it’s not as common. Kids with certain issues, like chronic constipation or bowel problems, might get it.
The focus for these children is on treating the root cause.
How does rectal prolapse affect a person’s quality of life?
It can make life tough, causing pain and social awkwardness. It interrupts daily life and can affect relationships.
However, timely medical care and treatment can greatly help.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.





