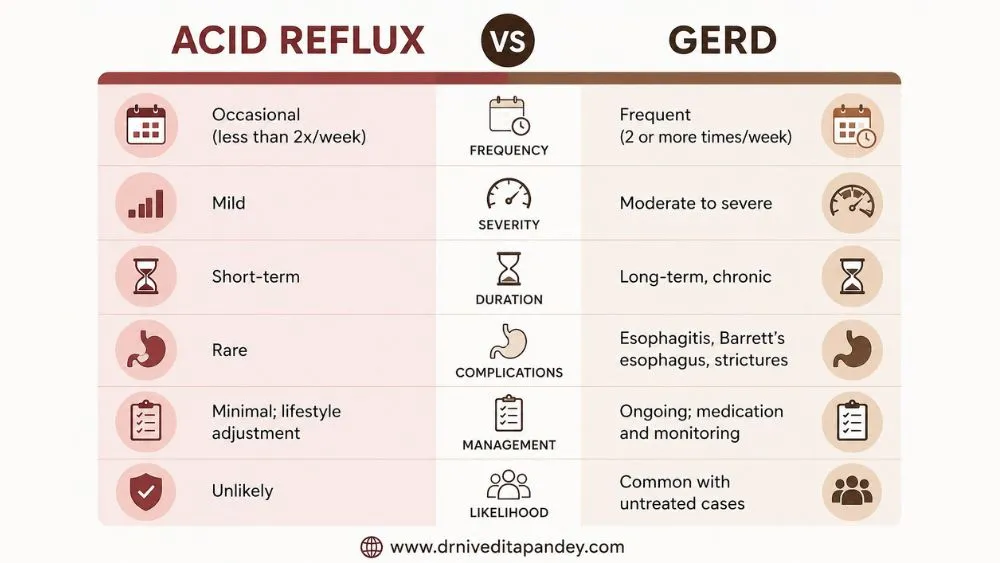
The difference between GERD and acid reflux is frequency and damage. Acid reflux is occasional, acid backs up into the esophagus and causes temporary discomfort. GERD is when that becomes a chronic pattern, happening at least twice a week, with real tissue damage over time.
Table of Contents
ToggleAcid reflux is manageable with simple adjustments. GERD is a disease that requires consistent, long-term management. The line between the two is crossed when frequency increases, when tissue damage begins, and when daily life starts to change around the symptoms. Catching that shift early changes the outcome significantly.
What Is GERD Compared to Acid Reflux?
Acid reflux is a physical event. Stomach acid enters the food pipe (esophagus) because the valve between them, the lower esophageal sphincter (LES), opens when it should not. This happens to nearly everyone at some point, usually after a heavy or spicy meal.
GERD, gastroesophageal reflux disease, is a medical diagnosis. It applies when acid reflux happens frequently enough to cause measurable symptoms or damage. The American College of Gastroenterology defines GERD as reflux symptoms appearing two or more times per week.
The clinical distinction matters because:
- Occasional acid reflux does not damage the esophagus long-term
- GERD, left untreated, causes esophagitis, strictures, and Barrett’s esophagus
- GERD requires ongoing management; acid reflux often resolves with diet changes alone
Key Difference Between GERD and Acid Reflux
The difference between GERD and acid reflux in practical terms: acid reflux is something that happens after a bad meal. GERD is something that controls what you eat, how you sleep, and what medications you take daily.
| Feature | Acid Reflux | GERD |
| Frequency | Occasional (less than 2x/week) | Frequent (2 or more times/week) |
| Severity | Mild | Moderate to severe |
| Duration | Short-term | Long-term, chronic |
| Complications | Rare | Esophagitis, Barrett’s esophagus, strictures |
| Treatment need | Minimal; lifestyle adjustment | Ongoing; medication and monitoring |
| Esophageal damage | Unlikely | Common with untreated cases |
Acid Reflux vs GERD Symptoms
The symptoms of acid reflux vs GERD are similar in type but different in intensity and persistence.
Acid Reflux Symptoms
- Heartburn after a specific trigger meal (spicy, fatty, or large portion)
- Mild sour or bitter taste in the mouth
- Discomfort lasting 30 minutes to 2 hours
- Symptoms clear on their own or with a single antacid
GERD Symptoms
- Persistent heartburn that returns daily or multiple times per week
- Regurgitation of food or liquid into the throat
- Difficulty swallowing, food feeling stuck in the chest
- Chronic cough without any respiratory cause
- Hoarse voice, especially in the morning
- Worsening symptoms at night regardless of what was eaten
Occasional acid reflux rarely disrupts sleep. GERD frequently does, because acid sits in the esophagus for hours during sleep, with no saliva production to buffer it and no upright posture to help gravity.
Persistent Cough: GERD vs Acid Reflux
Acid reflux causes temporary throat irritation. The cough clears once the reflux episode ends, usually within a few hours.
GERD causes a chronic dry cough that does not respond to cough syrup, antihistamines, or standard respiratory treatment. The reason: acid reaches the airway and irritates the larynx repeatedly over days, weeks, and months. The larynx becomes chronically inflamed.
Persistent cough GERD vs acid reflux by timeline:
- Acid reflux cough: lasts hours, tied to a specific meal or position
- GERD cough: lasts weeks to months, present regardless of meal timing, often worse at night and in the morning
In a 2006 study published in Chest , chronic cough linked to GERD accounted for up to 40% of chronic cough cases referred to pulmonologists. Most of those patients were initially treated for asthma or upper respiratory infection.
If a cough lasts more than 3 weeks with no respiratory cause, GERD is a likely driver.
Triggers of Acid Reflux vs GERD Progression
Acid reflux has clear, food-based triggers. GERD develops from structural and chronic lifestyle factors.
Common Acid Reflux Triggers
- Spicy food (capsaicin slows gastric emptying)
- Large meals (stretch the stomach and increase LES pressure)
- Lying down within 2 hours of eating
- Caffeine, alcohol, chocolate, and mint (all relax the LES)
- Carbonated drinks (gas pressure pushes acid upward)
GERD Progression Factors
Triggers of acid reflux vs GERD progression at the disease level involve more than food:
- Weak LES over time: Repeated acid reflux episodes reduce LES muscle tone. The valve gets weaker with each bout of untreated reflux.
- Obesity: Abdominal fat applies constant upward pressure on the stomach. This is not a one-meal problem; it is a daily mechanical force.
- Hiatal hernia: A structural defect where part of the stomach slides above the diaphragm. This physically prevents the LES from functioning correctly.
- Chronic exposure to triggers: Someone who eats trigger foods daily and ignores symptoms pushes acid reflux toward GERD over months to years.
- Smoking: Nicotine weakens the LES and reduces saliva production, removing the body’s main acid buffer.
When Acid Reflux Becomes GERD
Acid reflux does not become GERD overnight. The transition is gradual and often silent. Here is what to watch for:
- Symptoms appear more than twice a week consistently for 4 to 8 weeks
- Antacids stop providing full relief; symptoms return within hours
- Symptoms appear even on days with no obvious trigger food
- Daily life changes: avoiding certain meals, sleeping propped up, skipping social events with food
- Visible signs: weight loss from avoiding food, hoarse voice every morning
The difference between GERD and acid reflux at this stage is that GERD now requires professional diagnosis. An endoscopy shows whether the esophagus lining has started to change. Waiting at this point increases the risk of Barrett’s esophagus significantly.
Complications of GERD
Untreated GERD causes three main complications:
- Esophagitis: Inflammation of the esophagus lining. Causes pain, bleeding ulcers, and difficulty eating. Acid exposure over weeks causes this, not years.
- Esophageal strictures: Scar tissue from repeated inflammation narrows the esophagus. Swallowing becomes progressively more difficult. Solid food becomes hard to pass before liquids are affected.
- Barrett’s esophagus: The esophagus lining changes to resemble intestinal tissue. This is a pre-cancerous condition. Around 10 to 15% of people with chronic GERD develop it. Barrett’s esophagus increases the risk of esophageal adenocarcinoma, a cancer that has grown over 600% in incidence in the US since the 1970s.
None of these complications develop from occasional acid reflux. All of them develop from unmanaged, chronic GERD.
Treatment Options for GERD vs Acid Reflux
Treatment options for GERD vs acid reflux differ in intensity and duration.
Acid reflux treatment:
- Avoid the specific trigger food or habit
- Antacids (Tums, Maalox) for fast relief
- H2 blockers (famotidine) for moderate episodes
- No daily medication needed
GERD treatment:
- Proton pump inhibitors (PPIs) like omeprazole or pantoprazole, taken daily before the first meal
- Long-term dietary modification, not just avoiding one food
- Sleep position changes: left-side sleeping with 6 to 8 inch head elevation
- Weight loss for patients with obesity-related GERD
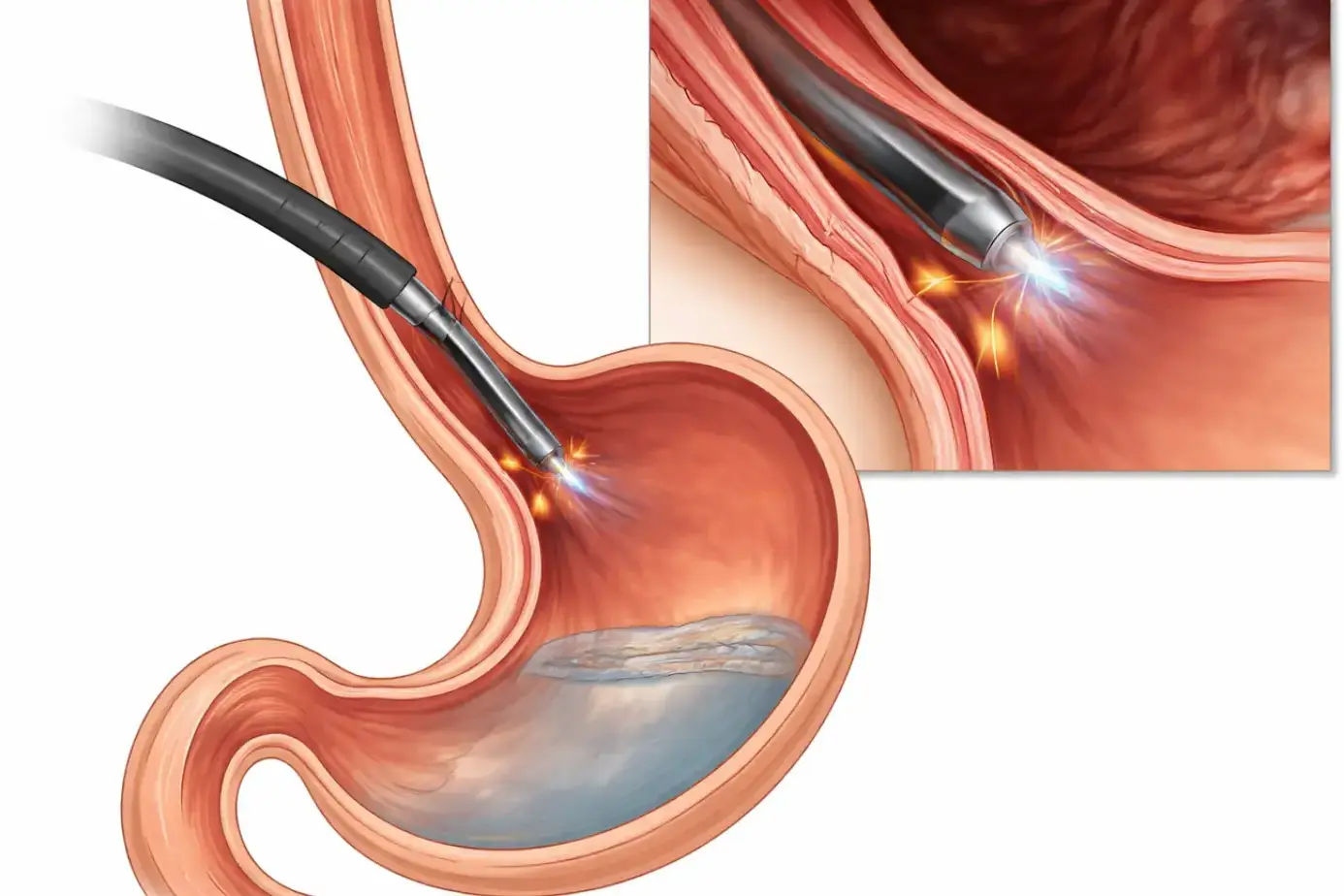
- Possible surgical treatment: Nissen fundoplication (wraps the stomach top around the LES) for patients who do not respond to medication
Treatment options for GERD vs acid reflux at the lifestyle level overlap. The difference is that acid reflux responds to occasional adjustments, while GERD requires a permanent, consistent plan. A person with acid reflux skips spicy food for a week. A person with GERD restructures their entire eating schedule, sleep setup, and medication routine.
When to See a Doctor
Do not wait if you experience:
- Heartburn or regurgitation more than twice a week
- Difficulty swallowing, even occasionally
- Unexplained weight loss
- A cough lasting more than 3 weeks with no respiratory cause
- Symptoms that do not improve after 2 weeks of OTC medication
- Vomiting blood or black stools
Any of these signs points to GERD. The difference between GERD and acid reflux at this stage is that self-treatment is no longer enough.
FAQs: Difference Between GERD and Acid Reflux
What is the main difference between GERD and acid reflux?
The difference between GERD and acid reflux is frequency and clinical classification. Acid reflux is a symptom that occurs occasionally. GERD is a diagnosed disease defined by acid reflux appearing two or more times per week, causing esophageal inflammation or measurable tissue damage over time.
Can acid reflux turn into GERD?
Yes. Repeated, untreated acid reflux weakens the LES muscle progressively. Once the LES loses enough tone, reflux becomes frequent and structural rather than trigger-based. This transition typically takes months to years of daily untreated reflux, especially in people who are obese or smoke.
Is GERD more serious than acid reflux?
Yes. Acid reflux causes temporary discomfort. GERD causes esophagitis, strictures, and Barrett’s esophagus. Barrett’s esophagus carries a measurable cancer risk. Unmanaged GERD increases the risk of esophageal adenocarcinoma, a cancer whose incidence has grown over 600% in the US since the 1970s.
Do both conditions cause heartburn?
Yes. Both cause heartburn, but the difference between GERD and acid reflux in this context is pattern. Acid reflux heartburn is tied to a specific trigger and clears within 2 hours. GERD heartburn returns daily, persists at night, and does not fully resolve with a single antacid.
Can GERD cause a cough?
Yes. Persistent cough GERD vs acid reflux separates at the 3-week mark. GERD causes a chronic dry cough from repeated acid reaching the larynx. Research in Chest found GERD responsible for up to 40% of chronic cough cases referred to lung specialists, most misdiagnosed as asthma initially.
Does acid reflux require treatment?
Occasional acid reflux does not require medication. Avoiding the trigger food resolves it. If it returns more than twice a week, or if antacids stop working within a few hours, that pattern needs medical evaluation to rule out GERD.
Can GERD be cured?
No permanent cure exists for GERD in most patients. Surgery (Nissen fundoplication) provides long-term relief in 85 to 90% of cases, but dietary discipline must continue post-surgery. PPIs control symptoms effectively but do not fix the structural LES weakness that causes GERD.
When should I worry about reflux?
Worry when symptoms appear more than twice a week, when swallowing becomes difficult, when you lose weight without trying, or when a dry cough persists for more than 3 weeks. These signs needs a gastroenterologist’s evaluation.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.