Acid reflux disease (GERD) is a chronic digestive condition where stomach acid repeatedly flows back into the esophagus. It is not the same as occasional heartburn after a spicy meal. When this happens more than twice a week, it is classified as GERD, and ignoring it causes real damage to the esophagus over time.
Table of Contents
ToggleGERD affects about 20% of adults in the US. GERD is manageable. To treat GERD naturally, start with weight, sleep, and food timing, three things that cost nothing but discipline. Add medication where needed and monitor long-term.
What Is GERD?
Acid reflux disease (GERD) stands for Gastroesophageal Reflux Disease. Your stomach has acid that breaks down food. Between the stomach and food pipe (esophagus), there is a muscular valve called the lower esophageal sphincter (LES). Its job is to stay closed after food enters the stomach.
In GERD, this valve either weakens or relaxes at the wrong time. Acid escapes upward. The esophagus has no protective lining against acid, so it gets irritated, inflamed, and damaged.
Acid reflux is when this happens occasionally. GERD is when it becomes a regular pattern with actual symptoms and tissue damage.
Common Symptoms of GERD
GERD symptoms and treatment decisions usually start from how often and how severely these symptoms appear:
- Heartburn , a burning sensation in the chest, usually after eating or when lying down. It gets worse at night.
- Acid regurgitation , the sour or bitter taste that rises into the throat or mouth.
- Dysphagia , difficulty swallowing. Food feels stuck in the chest or throat.
- Chronic cough , especially at night, without any respiratory cause. This one gets misdiagnosed frequently.
- Chest pain that mimics a heart attack. GERD-related chest pain is sharp, burning, and gets worse after meals.
GERD also causes laryngitis, hoarseness, and worsening asthma . Stomach acid that reaches the throat and airways triggers inflammation. Asthmatic patients with uncontrolled GERD have consistently worse lung function. The connection is well-documented in pulmonology research.
Some people have silent GERD , meaning no heartburn at all, just a persistent cough, hoarse voice, or the feeling of a lump in the throat. Silent GERD often goes undiagnosed for years.
What Causes GERD?
Causes of acid reflux and GERD comes down to pressure, anatomy, and lifestyle choices, often all three at once.
- Weak LES: The valve loses its muscle tone. Alcohol, smoking, and fatty foods all weaken it directly.
- Hiatal hernia: Part of the stomach pushes through the diaphragm into the chest cavity. This physically disrupts the LES, making acid reflux almost unavoidable. Hiatal hernia is present in the majority of people with severe GERD.
- Delayed gastric emptying: Food stays in the stomach longer than normal. The longer it sits, the higher the pressure, and the more likely acid is to push back up.
- Obesity: Extra abdominal fat increases pressure on the stomach constantly. Even a 10-15 pound weight gain can trigger or worsen GERD in someone who never had it before.
- Trigger foods and habits: Late-night eating, large meals, lying down immediately after eating, chocolate, caffeine, tomatoes, mint, and carbonated drinks are the most common culprits.
Risk Factors for GERD
GERD symptoms in adults are more common in people with these risk factors:
- BMI over 25 (overweight) or over 30 (obese)
- Pregnancy, because the growing uterus pushes stomach contents upward
- Active smoking, which directly weakens LES muscle tone
- Medications like calcium channel blockers, antihistamines, sedatives, and some antidepressants, all of which relax the LES
- Diets heavy in processed food, red meat, and saturated fat
Connective tissue disorders like scleroderma severely affect esophageal motility and are a major risk factor for both GERD and its worst complication, Barrett’s esophagus.
How GERD Is Diagnosed
Doctors begin with symptom history. If classic heartburn and regurgitation appear more than twice a week, a trial of proton pump inhibitors (PPIs) is usually prescribed. If symptoms improve, GERD is confirmed.
Diagnostic Tests
- Upper endoscopy (EGD): A thin camera goes down the throat to check for inflammation, ulcers, strictures, or Barrett’s esophagus. The gold standard for seeing actual damage.
- Ambulatory pH monitoring: A small probe measures acid levels in the esophagus over 24 to 48 hours. This catches acid exposure at different times, including during sleep.
- Esophageal manometry: Measures how well the esophagus muscles move and whether the LES pressure is abnormally low. This test is required before surgical treatment is considered.
Treatment Options for GERD
GERD symptoms and treatment overlap significantly because some of the best treatments are behavioral, not pharmaceutical.
Lifestyle Modifications
- Lose weight. A 2006 study in the New England Journal of Medicine confirmed that BMI reduction directly reduced GERD frequency.
- Elevate the head of your bed by 6 to 8 inches. Extra pillows do not work; bed wedges or bed risers do.
- Stop eating 2 to 3 hours before bed.
- Sleep on your left side. Right-side sleeping increases acid exposure because of how the stomach sits anatomically.
Dietary Changes
Best diet for GERD patients focuses on low-acid, low-fat foods eaten in smaller portions:
- Avoid: fried food, chocolate, coffee, citrus, tomato-based products, peppermint, carbonated drinks, alcohol
- Prefer: oatmeal, lean protein, non-citrus fruits (bananas, melons), green vegetables, ginger, alkaline water
- Eat 4 to 5 smaller meals instead of 2 to 3 large ones. Large meals expand the stomach and pressure the LES.
Foods to avoid with GERD are high-fat foods delay stomach emptying, which keeps acid pressure high for hours after eating.
Medications
- Antacids (Tums, Maalox): Neutralize acid fast. Relief lasts 1 to 2 hours. Not for daily use.
- H2 blockers (famotidine, ranitidine): Reduce acid production. Work within 1 hour. Good for mild-moderate GERD.
- Proton Pump Inhibitors (PPIs) (omeprazole, pantoprazole, esomeprazole): Block acid at the source. Most effective for healing esophageal damage. Take 30 to 60 minutes before the first meal for maximum effect.
Surgical and Advanced Treatments
GERD treatment without medication at the surgical level is an option when medications fail or cause side effects.
- Nissen fundoplication: The top of the stomach is wrapped around the lower esophagus and sewn in place to reinforce the LES. 85 to 90% of patients see significant improvement.
- LINX device: A ring of magnetic beads placed around the LES. It opens when you swallow, then closes again. Less invasive than fundoplication.
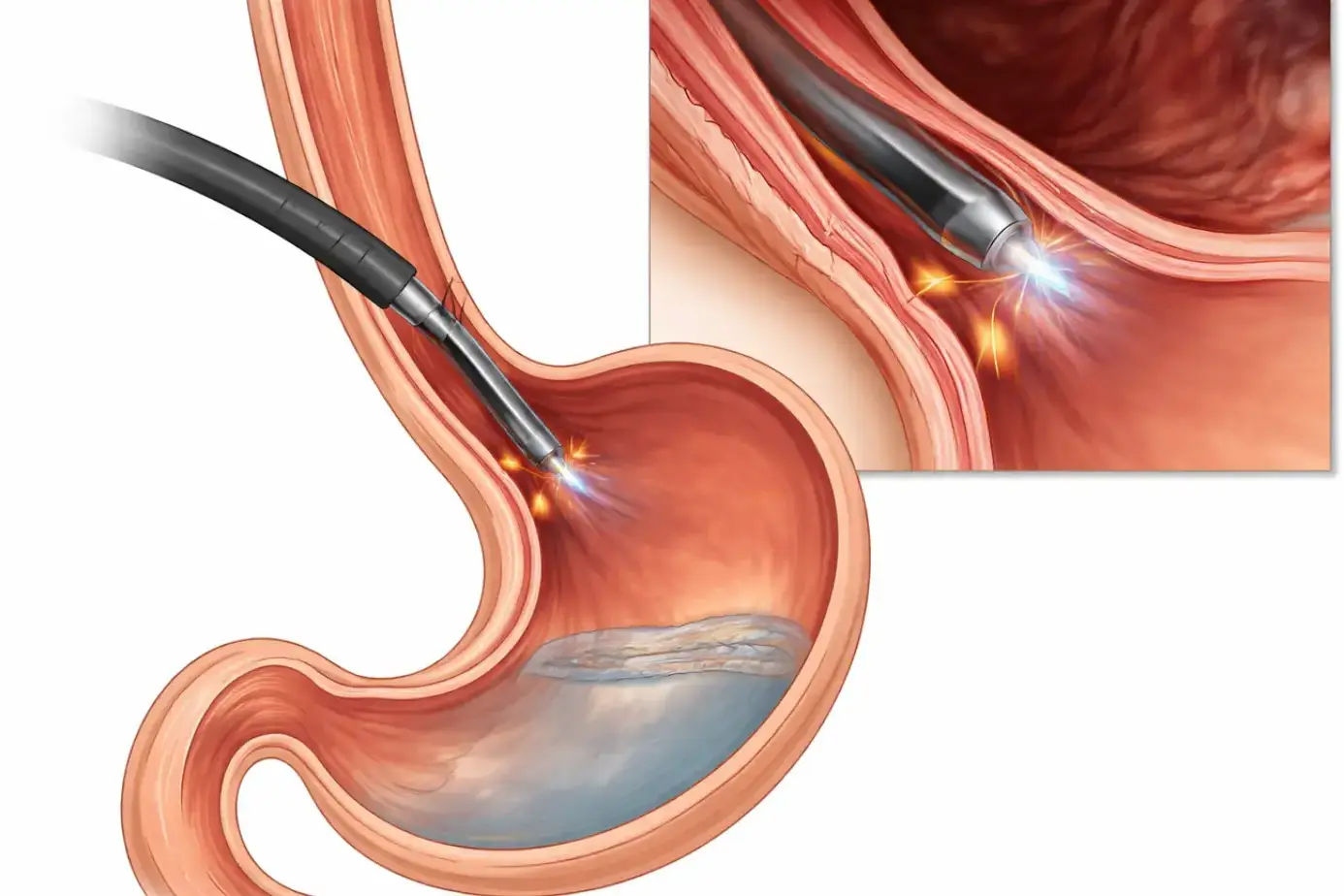
- Transoral incisionless fundoplication (TIF): An endoscopic procedure with no external incisions.
Complications of Untreated GERD
Long-term effects of GERD go far beyond daily discomfort:
- Esophagitis: Chronic inflammation. Causes pain, bleeding, and ulcers.
- Esophageal strictures: Scar tissue narrows the esophagus. Swallowing becomes progressively harder.
- Barrett’s esophagus: The lining of the esophagus changes to resemble intestinal tissue. This is a pre-cancerous condition. 10 to 15% of chronic GERD patients develop it.
- Esophageal adenocarcinoma: The cancer risk from untreated Barrett’s esophagus is real. It has increased by over 600% in the US since the 1970s, largely due to rising GERD rates.
Preventing GERD Symptoms
Treat GERD naturally and prevent recurrence comes down to consistency:
- Maintain a healthy BMI.
- Avoid smoking; nicotine relaxes the LES within minutes of a cigarette.
- Limit alcohol to reduce LES tone degradation.
- Sleep on the left side with the head elevated.
- Chew food slowly and thoroughly. Rushed eating increases swallowed air and stomach pressure.
- Avoid tight clothing around the waist, it literally compresses the stomach.
When to See a Doctor
Do not wait if you have:
- Symptoms more than twice a week despite dietary changes
- Difficulty swallowing, even occasionally
- Unintended weight loss
- Vomiting blood or black stools
- Chest pain (always rule out cardiac causes first)
- Symptoms not responding after 2 weeks of OTC medications
Long-Term Outlook
Acid reflux disease (GERD) is chronic for most people. It does not go away permanently without sustained changes. Even after surgery, dietary habits need to stay consistent.
Patients on long-term PPIs need periodic monitoring. PPI use beyond 1 year is linked to reduced magnesium absorption, increased risk of C. difficile infection, and in some studies, higher fracture risk. This does not mean stopping PPIs without a doctor, it means using the lowest effective dose and reassessing every 6 to 12 months.
With the right combination of lifestyle changes, medications, and monitoring, most people with GERD control their symptoms well. The ones who do not are usually the ones who treat it like heartburn and skip the follow-up.
Frequently Asked Questions About GERD
Can GERD be cured permanently?
No. GERD is a structural or functional problem with the LES. Lifestyle changes and surgery reduce symptoms significantly, but the underlying susceptibility remains. Around 62% of post-surgical patients maintain long-term relief without medication, but ongoing dietary habits still determine outcomes.
How is GERD different from acid reflux?
The acid reflux vs GERD difference is frequency and damage. Acid reflux is occasional. GERD symptoms apply when reflux occurs more than twice a week and causes measurable tissue damage or daily symptoms. Every GERD case involves acid reflux, but not every acid reflux case is GERD.
What foods should be avoided in GERD?
Foods to avoid with GERD: chocolate, coffee, alcohol, fried food, citrus, tomatoes, mint, and carbonated drinks. Chocolate is the worst offender because it both relaxes the LES and increases acid production simultaneously.
Are PPIs safe for long-term use?
PPIs are safe when used correctly, but long-term use beyond 12 months without reassessment carries risks: low magnesium, vitamin B12 deficiency, and slightly higher fracture rates in post-menopausal women. Your doctor should review your PPI need every 6 months.
Can GERD cause chest pain?
Yes. GERD symptoms and treatment for chest pain is more common than most people expect. GERD-related chest pain comes from esophageal spasms triggered by acid. It mimics cardiac chest pain closely enough that emergency rooms routinely run cardiac workups first. Always rule out heart causes before attributing chest pain to acid reflux disease (GERD).
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.