Cholangitis and cholecystitis often confuse patients because both involve the biliary system and can present with abdominal pain and fever. Yet, they are different problems requiring different treatments. Knowing the difference between cholangitis and cholecystitis is vital because delay in diagnosis can quickly turn life-threatening.
Table of Contents
ToggleThis detailed guide will help you understand both conditions, their causes, warning signs, treatments, complications, and preventive strategies in a way that is simple yet medically accurate.
Cholangitis Symptoms, Causes, and Treatments
What Is Cholangitis and How Does It Develop
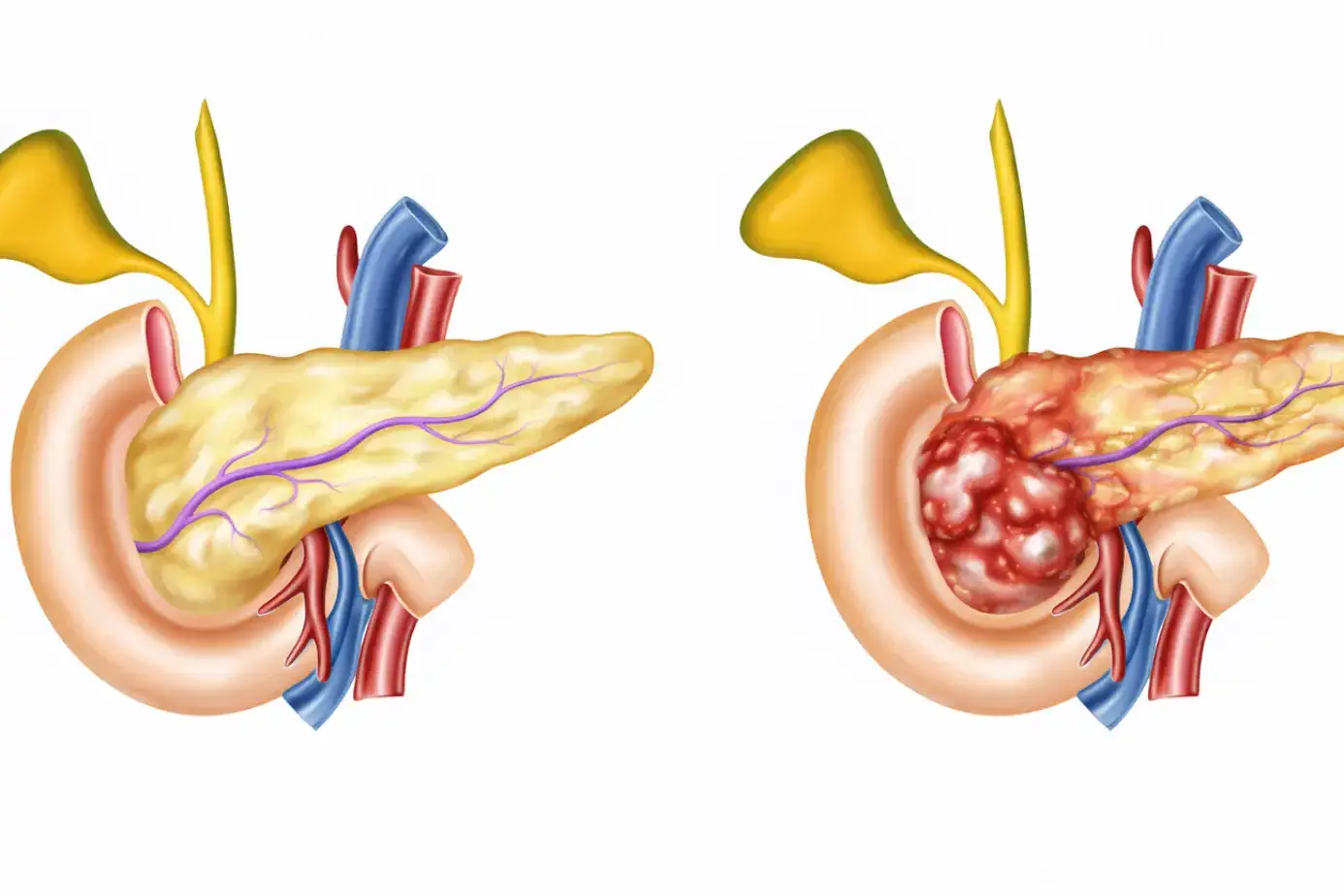
Cholangitis is an infection of the bile ducts. The bile ducts act like plumbing pipes, carrying bile from the liver to the small intestine. If these ducts get blocked, bile builds up. Stagnant bile creates the perfect environment for bacteria to grow, leading to infection known as biliary tract infection.
A common type is ascending cholangitis, where bacteria travel upward from the intestine into the bile ducts. When this happens, patients often get very sick, very fast.
Cholangitis Symptoms You Should Not Ignore
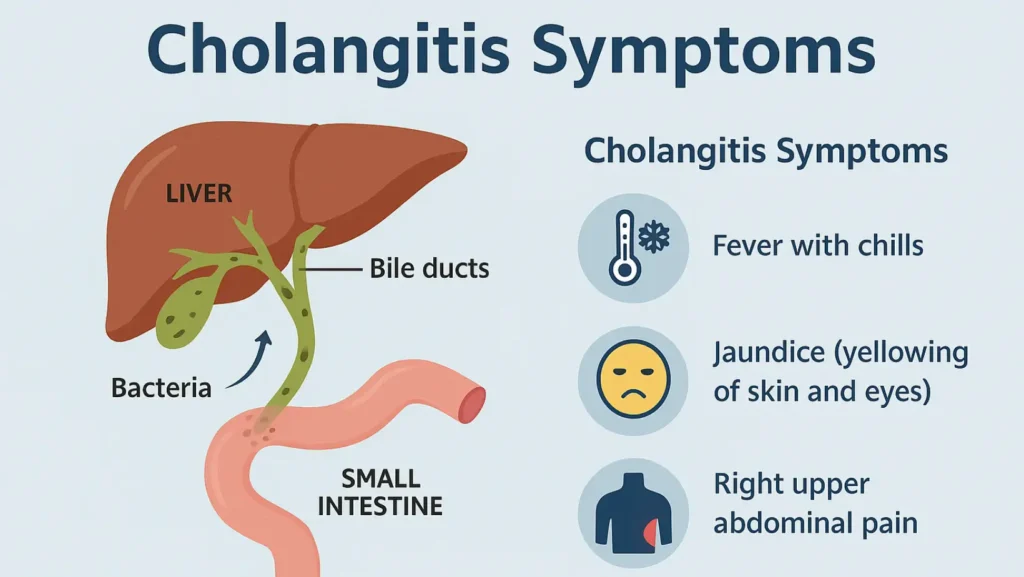
Classic cholangitis symptoms include:
- Fever with chills
- Jaundice (yellowing of skin and eyes)
- Right upper abdominal pain
These three make up Charcot’s triad cholangitis. If confusion and low blood pressure are added, it becomes Reynolds’ pentad, which signals severe infection and possible sepsis.
Other warning signs may include dark urine, pale stools, nausea, and vomiting. Patients sometimes report sudden worsening after a heavy meal.
Causes Of Cholangitis And Common Risk Factors
The most common causes of cholangitis include:
- Gallstones blocking the bile duct
- Narrowing of bile ducts due to previous surgery, injury, or scarring
- Tumors pressing on the duct
- Parasitic infections in endemic regions
- After ERCP or stent placement, where bacteria may gain entry
Risk factors include older age, prior bile duct surgery, liver disease, diabetes, and weakened immunity.
Treatment Options For Cholangitis
Treatment focuses on two goals:
- Control infection with IV antibiotics and fluids
- Relieve obstruction in the ducts
Antibiotics are started right away. Once the patient is stable, doctors often perform endoscopic retrograde cholangiopancreatography (ERCP) to remove stones or place stents. If ERCP is not possible, a percutaneous drain or surgery may be required.
Patients with low blood pressure or organ failure need intensive care. Quick recognition and urgent intervention save lives.
Cholecystitis Symptoms, Causes, and Treatments
What Is Cholecystitis And How Is It Different From Cholangitis?
Cholecystitis means gallbladder inflammation. The gallbladder is a small sac under the liver that stores bile. If a stone blocks its outlet, bile becomes trapped, leading to swelling, infection, and pain.
The key difference between cholangitis and cholecystitis is that cholecystitis affects the gallbladder only, while cholangitis affects the ducts carrying bile.
Cholecystitis Symptoms To Look Out For
Typical cholecystitis symptoms include:
- Steady right upper abdominal pain, often after fatty meals
- Fever
- Nausea and vomiting
- Tenderness under the right ribs
A classic sign during examination is Murphy’s sign cholecystitis. When a doctor presses under the ribs and asks the patient to breathe in, the sudden pain stops the breath midway.
Causes Of Cholecystitis And Gallbladder Inflammation
Most causes of cholecystitis are linked to gallstones blocking the cystic duct. This is why we say gallstones and cholecystitis often go hand in hand.
Other rare causes include infection without stones (acalculous cholecystitis), trauma, tumors, or poor blood supply. Risk rises in women over 40, obese individuals, people with rapid weight loss, or those on long-term IV feeding.
Treatment Options For Cholecystitis
Initial treatment involves IV fluids, pain relief, and antibiotics. Once stable, most patients undergo laparoscopic gallbladder removal (cholecystectomy).
If surgery is unsafe, doctors may place a tube into the gallbladder to drain pus and bile. This provides temporary relief until surgery becomes safe.
Key Points
- Cholangitis = infection of bile ducts.
- Cholecystitis = inflammation of gallbladder.
- Both need urgent care, but the definitive treatments differ.
Similarities Between Cholangitis and Cholecystitis
Detailed Notes
Both conditions cause right upper abdominal pain, fever, and nausea. Both may arise from gallstones. Blood tests show raised white blood cells and liver enzymes.
But the treatment target differs: duct clearance in cholangitis, gallbladder removal in cholecystitis. Recognizing these differences ensures timely action.
Cholangitis vs Cholecystitis: Understanding the Difference
The difference lies in the site of the problem. In cholangitis, the infection is in the ducts. In cholecystitis, it is in the gallbladder.
| Feature | Cholangitis | Cholecystitis |
| Definition | Infection of the bile ducts (bile duct inflammation) | Inflammation of the gallbladder (gallbladder inflammation) |
| Main Cause | Blockage of bile ducts (commonly by stones, strictures, or tumors) | Blockage of cystic duct, usually by gallstones |
| Classic Symptoms | Fever, jaundice, right upper abdominal pain (Charcot’s triad cholangitis) | Right upper abdominal pain, tenderness, fever, nausea (Murphy’s sign cholecystitis) |
| Pain Character | Diffuse right upper pain, sometimes with jaundice and chills | Steady, localized pain, worsens after fatty meals |
| Complications | Sepsis, liver abscess, multiple organ failure | Gallbladder rupture, empyema, gangrene |
| Lab Findings | Elevated liver enzymes, bilirubin, white blood cells | Elevated white blood cells, mild rise in liver enzymes |
| Imaging | Ultrasound or CT shows dilated bile ducts or stones | Ultrasound shows thickened gallbladder wall, stones, fluid |
| Definitive Test | ERCP confirms and treats blockage | HIDA scan (gold standard) if ultrasound unclear |
| Treatment | IV fluids, antibiotics, urgent duct clearance (ERCP or surgery) | IV fluids, antibiotics, gallbladder removal (cholecystectomy) |
| Prognosis | Life-threatening without urgent treatment | Usually favorable if treated promptly |
Diagnosis and Management of Acute Cholangitis
Symptoms of Acute Cholangitis
Acute cholangitis presents with fever, abdominal pain, and jaundice. Severe cases include confusion, shock, and rapid heart rate.
Diagnosis of Acute Cholangitis
Diagnosis combines blood tests and imaging. Blood tests show infection and liver dysfunction. Ultrasound or CT shows duct dilation or stones. ERCP confirms and treats the block.
Management of Acute Cholangitis – Summary
- Start IV fluids and antibiotics immediately.
- Relieve duct obstruction through ERCP or drainage.
- Provide ICU support in unstable patients.
Diagnosis and Management of Acute Cholecystitis

Symptoms of Acute Cholecystitis
Acute cholecystitis often presents as constant upper right abdominal pain lasting more than 6 hours. Fever and vomiting are common.
Diagnosis of Acute Cholecystitis
Ultrasound is the first test. It shows a thickened gallbladder wall, fluid around it, and stones. If unclear, a HIDA scan confirms blockage.
Treatment of Acute Cholecystitis
Standard treatment is laparoscopic cholecystectomy. Early removal prevents complications. In very ill patients, gallbladder drainage may be done first.
Key Points
- Use ultrasound to confirm diagnosis.
- Treat with fluids, antibiotics, and surgery.
Complications and Prognosis of Cholangitis vs Cholecystitis
Untreated cholangitis can lead to sepsis, abscesses, and death. Untreated cholecystitis can cause gallbladder rupture, gangrene, or abscess.
Prognosis improves with early intervention. Delay increases mortality.
Risk Factors for Cholangitis and Cholecystitis
Risk Factors for Cholangitis
- Gallstones in the duct
- Bile duct strictures
- Prior ERCP or surgery
- Tumors blocking the duct
- Weak immune system
Risk Factors for Cholecystitis
- Female, over 40, obese, fertile (the 5 Fs risk rule)
- Diabetes and metabolic syndrome
- Rapid weight loss
- Prolonged fasting or IV nutrition
Prevention of Cholangitis and Cholecystitis
Maintain a Healthy Lifestyle
Eat balanced meals and exercise. Steady weight prevents stone formation.
Avoid Excessive Alcohol Consumption
Alcohol damages liver cells and worsens bile flow. Moderation helps reduce risks.
Practice Safe Sex
Some infections like hepatitis spread through unsafe sex. They indirectly affect bile flow and increase risk.
Lifestyle Modifications for Gallstone Prevention
Eat fiber-rich foods, avoid crash diets, and maintain hydration. Regular exercise reduces gallstone risk.
Complications of Gallstones: Cholangitis and Cholecystitis
Complications of Gallstones
Gallstones can block ducts causing cholangitis or block the gallbladder causing cholecystitis. In rare cases, they pass into the bowel causing obstruction.
The Bottom Line
Both cholangitis and cholecystitis are emergencies that start with gallstones but affect different parts of the biliary system. Early recognition, antibiotics, and surgical or endoscopic interventions are key.
Delaying care may lead to severe infection, sepsis, or organ damage. Knowing the warning signs and seeking help quickly can make all the difference.
FAQs
How can you tell the difference between cholangitis and cholecystitis?
Cholangitis presents with fever, jaundice, and duct infection. Cholecystitis causes right-sided pain and gallbladder swelling. Imaging confirms diagnosis and guides treatment.
What is the triad of cholangitis?
Charcot’s triad cholangitis includes fever, right upper abdominal pain, and jaundice. This classic triad helps identify acute duct infection early.
What are the 5 F’s of cholecystitis?
The five F’s stand for female, forty, fertile, fat, and fair. These describe common risk factors for gallstone-related gallbladder problems.
How to confirm cholangitis?
Doctors confirm cholangitis using blood tests, imaging, and ERCP. ERCP not only diagnoses but also clears duct obstruction.
How to differentiate between cholelithiasis and cholecystitis?
Cholelithiasis means stones in the gallbladder. Acute cholecystitis means inflammation. Lasting pain, fever, and Murphy’s sign indicate inflammation.
What is the gold standard for cholecystitis?
Ultrasound is the first test. If unclear, a HIDA scan is considered the gold standard for diagnosing gallbladder blockage.
What IV antibiotics are used for cholecystitis?
Doctors often use piperacillin-tazobactam, or a third-generation cephalosporin with metronidazole. Choice depends on severity and local antibiotic guidelines.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.