Welcome to our article on achalasia of the esophagus. You may be dealing with this rare swallowing disorder if you have been experiencing difficulty swallowing, regurgitation, or chest pain. This article will explore the symptoms, causes, and treatment options for achalasia. Whether you seek information or solutions, we have you covered.
Table of Contents
ToggleWhat is Achalasia Of Esophagus?
Achalasia is a rare swallowing disorder that affects the esophagus and the lower esophageal sphincter. It is characterized by the inability of the esophagus muscles to contract correctly, leading to difficulty in moving food towards the stomach. The lower esophageal sphincter fails to relax, preventing food from entering the stomach. Achalasia typically affects adults between the ages of 30 and 60, with men being more commonly affected than women.
When you have achalasia, the muscles in your esophagus do not work as they should. The esophagus is the tube that carries food and liquids from your throat to your stomach. Usually, the muscles push food down through the esophagus and into the stomach. However, with achalasia, the muscles in the lower part of the esophagus do not relax as they should. This prevents food and liquids from entering the stomach correctly, causing swallowing difficulties.
| Key Features of Achalasia | Primary Symptoms |
|---|---|
| Esophagus | Difficulty in moving food towards the stomach |
| Lower Esophageal Sphincter | Failure to relax, leading to food blockage |
| Affected Population | Adults (30-60 years), more common in men |
If you have achalasia, you may experience symptoms such as difficulty swallowing, regurgitation of food or liquid, heartburn, chest pain, coughing, and weight loss. These symptoms can significantly impact your quality of life and daily activities. It is essential to seek medical attention if you suspect you may have achalasia.
The following section will explore the possible causes of achalasia and the factors contributing to its development.
Causes of Achalasia
The exact causes of achalasia are still unknown, but several theories have been proposed.
- Nerve cell degeneration: One theory is that achalasia may be caused by degeneration of the nerve cells in the esophageal muscles. This degeneration leads to the muscles’ inability to contract properly, affecting the movement of food through the esophagus.
- Autoimmune disorder: Another theory suggests that achalasia may be an inflammatory autoimmune disorder. In this case, the body’s immune system mistakenly attacks the nerve cells in the esophagus, leading to the dysfunction of the esophageal muscles.
- Viral infection: Some evidence also links achalasia to viral or parasitic infections. These infections may trigger an immune response or directly affect the nerve cells in the esophagus, contributing to the development of achalasia.
While these theories provide insights into the potential causes of achalasia, more research is needed to establish a definitive answer.
Summary of Achalasia Causes
| Cause | Description |
|---|---|
| Nerve cell degeneration | Degeneration of nerve cells in the esophageal muscles |
| Autoimmune disorder | Inflammatory immune response targeting nerve cells in the esophagus |
| Viral infection | Association with viral or parasitic infections impacting esophageal nerve cells |
Symptoms of Achalasia
Symptoms of achalasia usually occur during or after eating. The most common symptom is difficulty swallowing, where food or liquid feels stuck in the esophagus. Other symptoms include regurgitation of food and liquid, chest pain, heartburn, coughing (especially at night), and choking or inhaling food or fluid into the airways. These symptoms can be severe and may lead to weight loss, fatigue, and even pneumonia in some cases.
Common symptoms of achalasia include:
- Difficulty swallowing
- Regurgitation of food and liquid
- Chest pain
- Heartburn
- Coughing (especially at night)
- Choking or inhalation of food or liquid into the airways
Diagnosis of Achalasia
To diagnose achalasia, doctors may conduct various tests to assess the condition of the esophagus and identify abnormalities. These tests include:
- Esophageal Manometry: This test measures and records changes in pressure throughout the esophagus. A thin tube with sensors is inserted through the nose into the esophagus to measure muscle contractions and identify any food movement issues.
- Upper Endoscopy: During this procedure, a thin, flexible tube called an endoscope is inserted through the throat to examine the esophagus and stomach. A camera attached to the endoscope allows the doctor to inspect the internal structures and detect any abnormalities visually.
- Barium Swallow: This test involves the ingestion of a contrast medium containing barium, followed by X-ray imaging of the upper gastrointestinal tract. The barium coats the esophagus, highlighting any functional or structural abnormalities that may hinder food movement.
Together, these tests help doctors determine the location and severity of muscle contractions in the esophagus, aiding in accurately diagnosing achalasia.
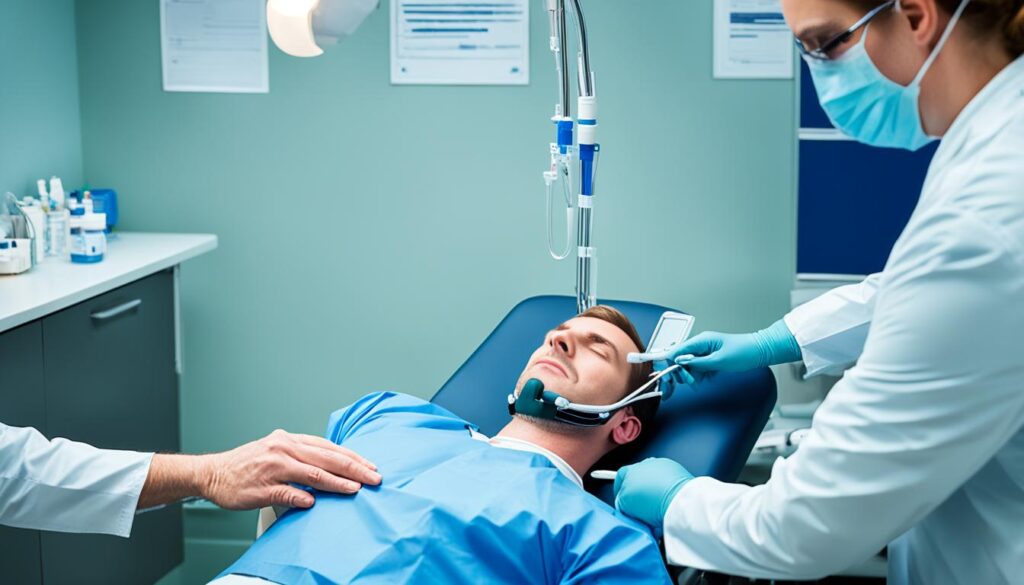
| Diagnostic Tests | Advantages | Disadvantages |
|---|---|---|
| Esophageal Manometry | – Measures and records pressure changes in the esophagus – Provides detailed information on muscle contractions – Helps differentiate achalasia from other esophageal disorders | – Requires insertion of a tube through the nose or mouth – May cause discomfort or irritation during the procedure |
| Upper Endoscopy | – Allows direct visualization of the esophagus and stomach – Helps detect abnormalities or structural issues – Can aid in obtaining biopsies if necessary | – Requires sedation or local anesthesia in some cases – Potential risk of complications like bleeding or perforation (rare) |
| Barium Swallow | – Provides clear imaging of the upper gastrointestinal tract – Highlights structural abnormalities or functional issues | – Requires ingestion of contrast medium – Involves exposure to X-ray radiation |
These diagnostic tests play a crucial role in evaluating and confirming achalasia, enabling healthcare providers to determine the most appropriate treatment plan for individuals affected by this condition.
Treatment Options for Achalasia
If you have been diagnosed with achalasia, there are several treatment options available to help manage your condition. The treatment choice will depend on your symptoms’ severity and personal preferences. Below are the esophageal achalasia treatment options commonly used for achalasia:
Dilation
One option is dilation, which involves widening the esophageal sphincter using a balloon. During this procedure, a deflated balloon is inserted into your esophagus and then inflated, stretching the narrowed area. This helps to improve food passage and relieve swallowing difficulties.
Surgery
If dilation is not practical or suitable for you, achalasia surgery may be recommended. In a procedure called myotomy, the muscles in your esophagus are cut to relieve the obstruction. This surgical intervention aims to improve food movement through your esophagus and into your stomach.
Botulinum Toxin Injections
Another treatment option is botulinum toxin injections. This involves injecting the toxin into the lower esophageal sphincter to temporarily relax the muscles and allow food to pass more quickly. However, it’s important to note that the effects of botulinum toxin injections are temporary and may require repeated injections over time.
Medications
Medications such as nitrates or calcium channel blockers can be prescribed to help manage achalasia symptoms. These medications work by relaxing the muscles in the esophagus, making it easier for food to pass through. However, drugs are generally less effective than other treatment options and may only provide temporary relief.
Discussing these treatment options with your healthcare provider to determine the best course of action for your specific situation is essential. When recommending a treatment plan, they will consider factors such as the severity of your symptoms, your overall health, and your preferences. Remember, treatment for achalasia aims to improve your ability to swallow and enhance your quality of life.
In the table below, you can find a summary of the different treatment options for achalasia:
| Treatment Option | Description |
|---|---|
| Dilation | Widening the esophageal sphincter using a balloon |
| Surgery | Myotomy procedure to cut the esophageal muscles |
| Botulinum Toxin Injections | Injecting the toxin to temporarily relax the lower esophageal sphincter |
| Medications | Prescribed drugs to relax the esophageal muscles |
Living with Achalasia
While living with achalasia can present challenges, making specific diet and lifestyle modifications can help alleviate symptoms and improve your overall well-being. Although no particular diet is proven to treat achalasia, many individuals find that avoiding certain foods can make swallowing easier. Consider reducing or eliminating the consumption of raw fruits and vegetables, tough cuts of meat, highly acidic foods, alcohol, and caffeine.
Instead, opt for softer and easier-to-swallow foods. Chewing your food thoroughly and taking your time eating can also assist in swallowing. Eating smaller, more frequent meals can reduce the amount of food that needs to pass through your esophagus, minimizing discomfort.
Additionally, it is essential to pay attention to your eating habits throughout the day. Avoiding solid foods close to bedtime can help minimize nighttime symptoms, such as coughing and regurgitation. The goal is to create a routine and adopt habits that optimize your ability to swallow comfortably.
Everyone’s experience with achalasia is unique, so working closely with your healthcare provider to create a personalized diet and lifestyle plan that suits your needs is crucial. They can provide valuable guidance and recommendations tailored to your specific situation.
Sample Menu for Living with Achalasia
Here’s a sample menu that can serve as a starting point for individuals living with achalasia:
| Meal Time | Food Options |
|---|---|
| Breakfast |
|
| Morning Snack |
|
| Lunch |
|
| Afternoon Snack |
|
| Dinner |
|
| Evening Snack |
|
Note: Consult your healthcare provider or a registered dietitian before significantly changing your diet. They can provide professional dietary advice tailored to your specific needs.

Complications of Achalasia and Follow-Up
While there are treatment options available for achalasia to manage symptoms and improve quality of life, it is essential to be aware of potential complications that may arise. These complications can include:
- Esophageal Perforation: In some cases, stretching or manipulating the esophagus during treatment procedures, such as dilation or surgery, can lead to esophageal perforation, which is a tear or hole in the esophageal wall. This is a serious complication that may require immediate medical attention to avoid further complications.
- Lack of Treatment Success: Some individuals may not experience significant symptom relief or improvement after undergoing treatment for achalasia. This can occur due to various factors, such as the severity of the condition or individual differences in response to treatment methods.
- Gastroesophageal Reflux Disease (GERD): Achalasia can increase the risk of developing gastroesophageal reflux disease, a condition where stomach acid flows back into the esophagus, causing symptoms such as heartburn, regurgitation, and chest pain. Ongoing monitoring and management of GERD symptoms may be necessary.
- Bloating: Some individuals with achalasia may experience bloating and discomfort in the abdomen due to the buildup of food and gas in the esophagus and stomach. This can cause feelings of fullness and distension and can impact overall quality of life.
Long-term follow-up is essential in managing achalasia and monitoring for any potential complications or recurrence of symptoms. Your healthcare provider may recommend periodic tests and evaluations to ensure the esophagus is functioning correctly and to rule out the development of other conditions.
Types of Achalasia
Achalasia can be classified into different types based on how the esophageal muscles malfunction.
| Type | Description |
|---|---|
| Classic Achalasia (Type 1) | Minimal muscle contractions in the esophagus |
| Type 2 Achalasia | Increased pressure in the esophagus leading to compression |
| Spastic Achalasia (Type 3) | Abnormal contractions at the bottom of the esophagus |
Recent Advancements in Achalasia Treatment
Significant progress has been made in treating achalasia, a rare swallowing disorder. One of the recent advancements in achalasia treatment is the peroral endoscopic myotomy (POEM) procedure, which offers a minimally invasive surgical option.
The POEM procedure involves using an endoscope to access the esophagus and create a tunnel within the muscles, allowing for easier food passage. This innovative technique has shown promising results in improving symptoms. It has become an alternative to the traditional laparoscopic Heller myotomy.
With the POEM procedure, patients experience less pain and a faster recovery compared to traditional open surgery. This minimally invasive approach reduces the risk of complications and scarring, improving patient outcomes.
Other advancements in achalasia treatment are being explored to enhance patient care further. These advancements aim to optimize treatment options, minimize invasiveness, and improve long-term outcomes. The field of minimally invasive surgery continues to evolve, offering immense potential for achalasia patients.
Here’s a table summarizing the key differences between the POEM procedure and traditional laparoscopic Heller myotomy:
| Procedure | POEM Procedure | Laparoscopic Heller Myotomy |
|---|---|---|
| Approach | Endoscopic | Laparoscopic |
| Invasiveness | Minimally invasive | Minimally invasive |
| Pain | Less post-operative pain | Less post-operative pain |
| Recovery Time | Shorter recovery period | Shorter recovery period |
| Risk of Complications | Reduced risk | Reduced risk |
- With advancements like the POEM procedure, achalasia treatment continues to evolve, providing hope for improved outcomes and enhanced quality of life for patients. These developments in minimally invasive surgery mark an exciting time in the field, offering new options and improving the management of achalasia.
Conclusion
Achalasia is a rare swallowing disorder that can greatly impact one’s ability to eat and drink comfortably. Although there is no cure for achalasia, several treatment options are available to manage symptoms and improve one’s quality of life. These options include dilation, surgery, botulinum toxin injections, and medications.
Living with achalasia may require making dietary and lifestyle modifications to make swallowing easier. Avoiding certain foods, eating smaller and more frequent meals, and chewing food thoroughly can all help alleviate symptoms. Additionally, working closely with a healthcare provider to develop a personalized diet and lifestyle plan is essential.
Regular follow-up appointments with your healthcare provider are crucial to monitor potential complications and ensure your condition is effectively managed. With the proper treatment, support, and lifestyle adjustments, individuals with achalasia can find relief and lead fulfilling lives.
FAQ
What is achalasia of the esophagus?
Achalasia of the esophagus is a rare swallowing disorder that affects the muscles of the esophagus and the lower esophageal sphincter. It results in difficulty in moving food from the esophagus to the stomach.
What are the causes of achalasia?
The exact causes of achalasia are still unknown. Still, theories suggest that it may be caused by degeneration of nerve cells in the esophageal muscles, an inflammatory autoimmune disorder, or viral infections.
What are the symptoms of achalasia?
Symptoms of achalasia include difficulty swallowing, regurgitation of food or liquid, chest pain, coughing, heartburn, weight loss, and vomiting.
How is achalasia diagnosed?
Achalasia can be diagnosed through tests such as esophageal manometry, upper endoscopy, and barium swallow, which help analyze muscle contractions and detect abnormalities in the esophagus.
What are the treatment options for achalasia?
Treatment options for achalasia include dilation, surgery, botulinum toxin injections, and medications. Treatment choice depends on the severity of the condition and individual preferences.
How can I live with achalasia?
Individuals with achalasia can make dietary and lifestyle modifications, such as avoiding certain foods and eating smaller, more frequent meals, to make swallowing easier. Regular follow-up with a healthcare provider is essential to monitor potential complications and manage the condition.
What are the complications of achalasia, and how is it followed up?
Complications of achalasia treatment can include esophageal perforation, lack of treatment success, gastroesophageal reflux disease, and bloating. Long-term follow-up is necessary to monitor for symptom recurrence and potential complications.
What are the types of achalasia?
Achalasia can be classified into different types based on the way the esophageal muscles malfunction, including classic achalasia, Type 1, characterized by minimal muscle contractions in the esophagus, and spastic achalasia, Type 3, involving abnormal contractions at the bottom of the esophagus.
What are some recent advancements in achalasia treatment?
One recent advancement is the peroral endoscopic myotomy (POEM). This minimally invasive surgery has shown promising results in improving symptoms. Other advancements in achalasia treatment are currently being explored.
What is the conclusion regarding achalasia?
Achalasia is a rare swallowing disorder that can significantly impact a person’s ability to eat and drink comfortably. While there is no cure, treatment options are available to manage symptoms and improve quality of life. Working with healthcare providers to find the best approach for each individual is essential.
Source Links
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.





