Did you know that esophageal cancer is one of the fastest-growing cancers in the United States? According to the American Cancer Society, there were an estimated 19,000+ cases of esophageal cancer diagnosed in 2021 alone.*
Table of Contents
ToggleWhen it comes to fighting this aggressive disease, knowledge is power. In this comprehensive guide, we will delve into the various treatment options available for esophageal cancer, equipping you with the information you need to make informed decisions about your care and improve your chances of recovery.
Surgery as a Treatment for Esophageal Cancer
Surgery is a common and effective treatment option for esophageal cancer. Depending on the stage and location of the cancer, surgical procedures can involve the partial or complete removal of the esophagus (esophagectomy), accompanied by the reconstruction of the digestive system.
Esophageal cancer surgery aims to remove the tumor and nearby affected tissues to inhibit the spread of cancer cells further. It can be performed using different techniques, including:
1. Transhiatal Esophagectomy: In this procedure, the surgeon removes the tumor through incisions made in the neck and abdomen. The esophagus is then reconnected to the stomach. This approach may be preferred for tumors located in the lower part of the esophagus or gastroesophageal junction.
2. Transthoracic Esophagectomy: This surgery involves incisions in the abdomen and chest to access and remove the tumor. Depending on the case, a portion of the stomach or colon may be used to reconstruct the digestive system.
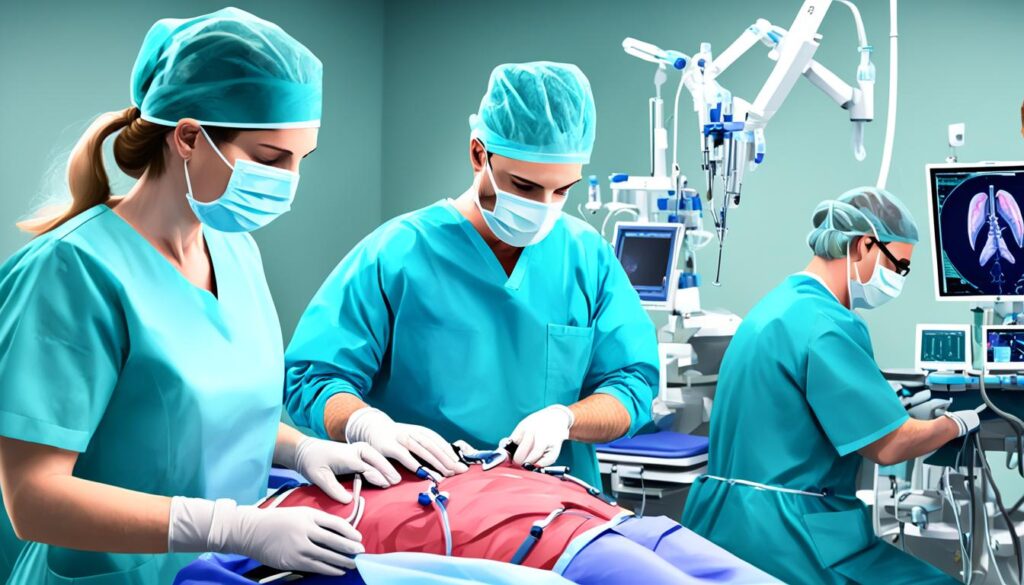
3. Minimally Invasive Esophagectomy: Also known as laparoscopic or robotic-assisted surgery, this technique involves small incisions and the use of specialized instruments and cameras. It offers the advantage of reduced surgical trauma, shorter hospital stays, and faster recovery times.
Surgical treatment for esophageal cancer may be recommended as the primary treatment or in combination with other therapies, such as chemotherapy and radiation therapy. The choice of surgical approach depends on various factors, including the cancer stage, location, and the patient’s overall health.
As with any surgery, there are risks and potential complications associated with esophageal cancer surgery, such as infection, bleeding, and damage to surrounding organs. However, advances in surgical techniques and perioperative care have significantly improved outcomes, leading to better quality of life and increased long-term survival rates.
Recovery and Follow-up Care
Recovery from esophageal cancer surgery can vary depending on the extent of the procedure and individual factors. Patients may experience discomfort, difficulty swallowing, or changes in diet during the initial recovery period. The healthcare team will provide guidance and support throughout the recovery process.
After surgery, regular follow-up appointments will be scheduled to monitor the patient’s progress, detect any potential complications, and ensure optimal recovery. These appointments may include imaging tests, endoscopic examinations, and discussions about post-operative care, such as dietary modifications and lifestyle adjustments.
Radiation Therapy for Esophageal Cancer
Radiation therapy is an essential treatment option for esophageal cancer. This approach utilizes high-energy beams to target and destroy cancer cells in the body. Radiation treatment for esophageal cancer can be conducted externally or internally, based on the specific needs of each patient.
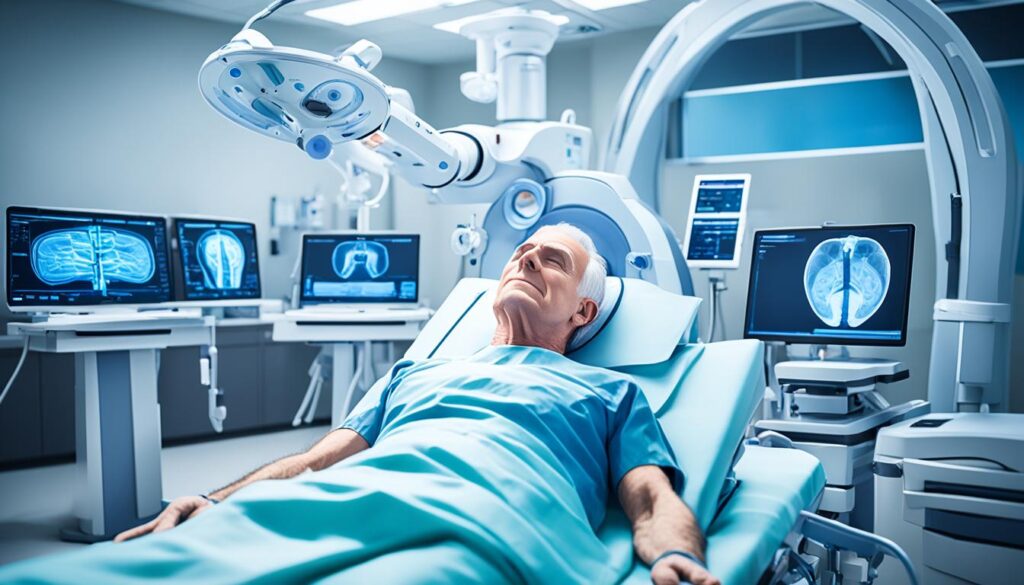
External Beam Radiation Therapy
The most common form of radiation therapy for esophageal cancer is external beam radiation therapy. During this procedure, a machine emits carefully directed beams of radiation towards the cancerous cells. The goal is to deliver a precise dose that kills the cancer cells while minimizing damage to surrounding healthy tissues. This form of radiation therapy is typically administered over a period of several weeks, with multiple sessions scheduled.
External beam radiation therapy has proven effective in shrinking tumors before surgery or reducing symptoms in advanced cases of esophageal cancer. However, it may cause side effects such as fatigue, difficulty swallowing, skin irritation, and nausea. Your healthcare team will closely monitor your progress and provide supportive care to manage any potential side effects.
Internal Radiation Therapy (Brachytherapy)
In some cases, internal radiation therapy, also known as brachytherapy, may be recommended. This procedure involves inserting a small radioactive device directly into or near the tumor. The device emits radiation, effectively killing the cancer cells. Internal radiation therapy is often used in conjunction with external beam radiation therapy to provide a more targeted treatment approach.
Brachytherapy can be delivered as a one-time treatment or over multiple sessions. This method allows for higher doses of radiation to be delivered directly to the tumor, while sparing healthy surrounding tissues. The most common side effects of brachytherapy include fatigue, mild pain or discomfort, and temporary difficulty swallowing.
| Advantages of Radiation Therapy for Esophageal Cancer | Potential Side Effects |
|---|---|
|
|
Chemotherapy for Esophageal Cancer
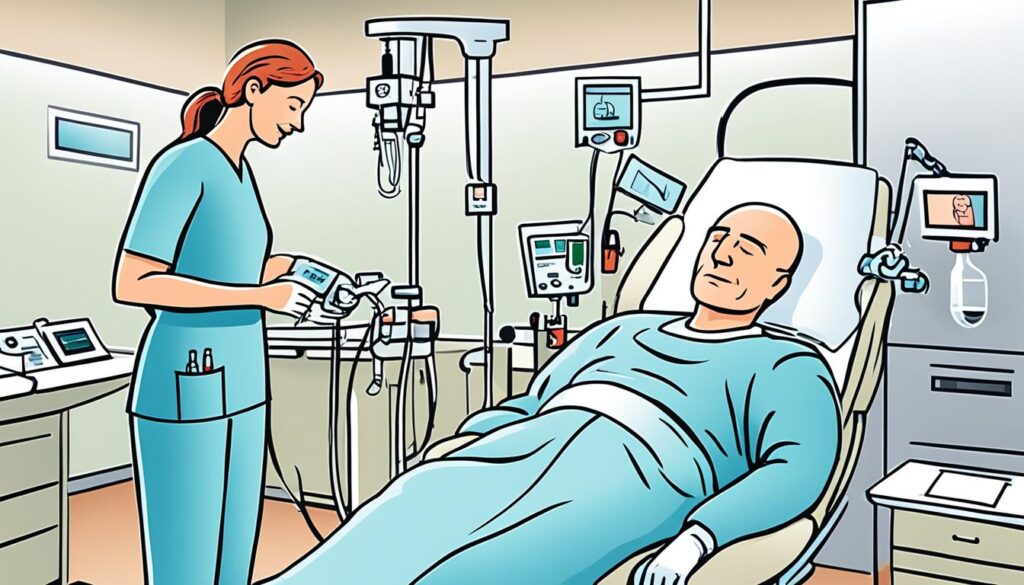
Chemotherapy is an integral component of esophageal cancer treatment. It involves the use of powerful drugs to target and destroy cancer cells throughout the body. Chemotherapy can be administered before surgery to shrink tumors, after surgery to eliminate any remaining cancer cells, or as the primary treatment option for advanced or metastatic esophageal cancer.
Chemotherapy drugs can be given orally, by injection, or through an intravenous drip. They enter the bloodstream and travel throughout the body, targeting cancer cells wherever they may be. By attacking cancer cells at a systemic level, chemotherapy helps to slow down the progression of the disease and improve overall outcomes.
Chemotherapy is often used in combination with other treatment modalities, such as surgery or radiation therapy, to enhance its effectiveness. This multidisciplinary approach can help increase the chances of successful treatment and improve the patient’s quality of life.
While chemotherapy is a powerful tool in fighting esophageal cancer, it can also cause side effects. The drugs used in chemotherapy can affect both cancer cells and healthy cells, leading to various temporary side effects. These side effects may include nausea, vomiting, fatigue, hair loss, and changes in blood counts. However, advancements in supportive care have helped reduce the severity of these side effects and improve patient comfort during treatment.
It is essential for patients undergoing chemotherapy to closely monitor their health and communicate any side effects to their healthcare team. This allows for timely intervention and adjustment of the treatment plan to minimize discomfort and optimize the effectiveness of chemotherapy.
Targeted Therapy for Esophageal Cancer
When it comes to the treatment of esophageal cancer, targeted therapy is emerging as a promising approach. Unlike traditional treatments that may affect healthy cells alongside cancer cells, targeted therapy specifically targets cancer cells, minimizing potential side effects.
Esophageal cancer targeted therapy involves using drugs or other substances that interfere with specific molecules involved in the growth and spread of cancer cells. These targeted treatments can be administered through oral medications or intravenous infusion.
One example of targeted therapy used in esophageal cancer treatment is the use of epidermal growth factor receptor (EGFR) inhibitors. These medications block the signals that promote cancer cell growth, ultimately slowing down or halting tumor progression.
Another targeted therapy approach is angiogenesis inhibitors. These drugs work by inhibiting the formation of new blood vessels that supply nutrients to cancer cells, thus preventing tumor growth and spread.
The effectiveness of targeted therapy in esophageal cancer treatment varies depending on individual cases. Some patients may experience substantial benefits, including tumor shrinkage, slowed tumor growth, and increased survival rates. However, it is important to note that not all patients respond equally to targeted treatments.
It is also worth mentioning that targeted therapy can be used in combination with other treatments, such as chemotherapy and radiation therapy, to enhance their outcomes. This comprehensive approach is known as multimodal therapy and aims to maximize the chances of successful treatment.
Advantages of Targeted Therapy for Esophageal Cancer
- Minimizes damage to healthy cells
- Potential for improved treatment outcomes
- Offers a personalized approach based on molecular characteristics
- Possibility of reducing side effects compared to traditional treatments
As research and clinical trials continue to advance, targeted therapy holds great promise for esophageal cancer treatment. It provides hope for patients who may not be suitable candidates for surgery or have already undergone traditional treatments.
Consulting with your healthcare team is essential to determine if targeted therapy is a viable option for your specific case. They can provide valuable insights into the potential benefits and risks associated with this treatment approach.
Immunotherapy for Esophageal Cancer
Immunotherapy is a revolutionary approach to treating esophageal cancer that harnesses the power of your own immune system to fight against cancer cells. This cutting-edge treatment has shown promising results and is quickly emerging as a valuable option for patients.
Unlike traditional cancer treatments such as surgery, radiation therapy, and chemotherapy, which directly target cancer cells, immunotherapy focuses on boosting the body’s natural defenses to recognize and destroy cancer cells.
How Does Immunotherapy Work?
Immunotherapy works by using substances called immune checkpoint inhibitors to block the proteins that prevent the immune system from recognizing and attacking cancer cells. By doing so, it enhances the immune response against cancer and helps to control its growth.
One of the most widely studied immune checkpoint inhibitors used in the treatment of esophageal cancer is pembrolizumab (Keytruda). This drug has shown significant efficacy in some patients, particularly those with advanced or metastatic esophageal cancer.
Potential Side Effects and Effectiveness
While immunotherapy offers great promise, it’s important to be aware of potential side effects. They can range from mild to severe and may include fatigue, rash, diarrhea, nausea, and immune-related adverse events. However, it’s vital to note that not all patients experience these side effects, and they can often be managed with proper medical care.
In terms of effectiveness, immunotherapy has demonstrated remarkable results in some patients with esophageal cancer. However, it’s important to remember that every individual’s response to treatment may vary, and not all patients may experience the same level of benefit.
The Role of Immunotherapy in Combination Treatments
Immunotherapy is often used in combination with other treatment modalities for esophageal cancer, such as chemotherapy and radiation therapy. This approach aims to maximize the therapeutic benefits by attacking cancer from multiple angles.
Combining immunotherapy with other treatments has shown promising results in improving overall response rates and survival outcomes. Ongoing research is also exploring the use of immunotherapy in combination with targeted therapies to further enhance treatment efficacy.
As the field of immunotherapy continues to advance, more exciting breakthroughs are expected in the treatment of esophageal cancer. By leveraging the body’s own immune system, immunotherapy provides renewed hope for patients battling this challenging disease.
Clinical Trials for Esophageal Cancer Treatment
Clinical trials play a crucial role in advancing the field of esophageal cancer treatment. They offer access to new and innovative therapies that have the potential to improve outcomes for patients. Participating in a clinical trial provides an opportunity to receive experimental treatments that may not be available through standard approaches.
By joining a clinical trial, you contribute to the development of future treatment options and help researchers gain valuable insights into the effectiveness and safety of these therapies. Clinical trials are designed with strict protocols and guidelines to ensure participant safety and ethical considerations.
The Importance of Clinical Trials
Clinical trials are vital for finding breakthroughs in esophageal cancer treatment. These trials evaluate the efficacy of new treatment options, such as targeted therapies, immunotherapies, and combination therapies.
Through clinical trials, researchers can assess the benefits and potential side effects of experimental treatments. This information is crucial for developing evidence-based guidelines for the management of esophageal cancer.
Finding Ongoing Trials
There are various ways to find ongoing clinical trials for esophageal cancer:
- Consult with your healthcare team: Your healthcare provider can provide information about clinical trials that may be suitable for your specific case.
- Search online databases: Websites such as ClinicalTrials.gov and the National Cancer Institute’s website provide comprehensive listings of active clinical trials.
- Contact research institutions: Reach out to prominent research institutions and cancer centers to inquire about ongoing trials.
When considering a clinical trial, it is essential to carefully review the eligibility criteria, potential risks, and benefits. Discuss your options with your healthcare team and loved ones before making a decision.
Potential Benefits and Risks
Participating in a clinical trial offers several potential benefits:
- Access to innovative treatments: Clinical trials provide access to experimental therapies that may offer improved outcomes.
- Contribution to scientific knowledge: By participating in a clinical trial, you contribute to medical research and help shape future treatment approaches.
- Close medical monitoring: Clinical trial participants receive regular medical check-ups and monitoring, ensuring their health is closely supervised.
However, it’s important to consider the potential risks and uncertainties associated with clinical trials:
- Possible side effects: Experimental treatments may have unknown side effects or adverse reactions.
- Lack of guaranteed benefit: There is no guarantee that the experimental treatment will be more effective than standard therapies.
- Time commitment: Clinical trials often require frequent visits to the research center and additional time commitment.
It’s essential to have open and honest conversations with your healthcare team about the potential risks and benefits of participating in a clinical trial. They can help you weigh the pros and cons and make an informed decision about what is best for your specific situation.
Current Clinical Trials
| Study Name | Description | Eligibility Criteria |
|---|---|---|
| Study 1 | Investigating the efficacy of a novel immunotherapy in patients with advanced esophageal cancer. | – Stage IV esophageal cancer – Good overall health – Previous treatment failure |
| Study 2 | Assessing the effectiveness of a targeted therapy combined with chemotherapy in neoadjuvant treatment for esophageal cancer. | – Locally advanced esophageal cancer – Fit for chemotherapy – No previous treatment |
| Study 3 | Exploring the safety and efficacy of a new radiation treatment modality for early-stage esophageal cancer. | – Stage I or II esophageal cancer – Medically fit for radiation therapy – No previous treatment |
These are just a few examples of the countless clinical trials currently ongoing for esophageal cancer treatment. It’s crucial to consult with your healthcare team and explore the options available to you.
Remember, participation in a clinical trial is entirely voluntary, and you have the right to withdraw at any time if you decide it’s no longer suitable for you.
Conclusion
In conclusion, when it comes to treating esophageal cancer, it is crucial to have a comprehensive understanding of the various treatment options available. From surgery to radiation therapy, chemotherapy to targeted therapy, and immunotherapy to clinical trials, advancements in medical science have provided promising avenues to increase the chances of recovery.
Consulting with your healthcare team is essential in determining the best treatment plan for you. They will consider factors such as the stage of your cancer, your overall health, and your individual needs. Working together, you can make informed decisions about your care that align with your goals and priorities.
Remember, staying informed about the latest developments in esophageal cancer treatment is key. By remaining proactive in your healthcare journey, you can explore all available options and maximize your chances of successful treatment and long-term survival.
FAQ
What are the treatment options for esophageal cancer?
The treatment options for esophageal cancer include surgery, radiation therapy, chemotherapy, targeted therapy, immunotherapy, and participation in clinical trials.
How is surgery used as a treatment for esophageal cancer?
Surgery is a common treatment for esophageal cancer and may involve removing part or all of the esophagus. The specific procedure will depend on factors such as tumor size, location, and stage of cancer.
What is radiation therapy and how is it used in esophageal cancer treatment?
Radiation therapy uses high-energy beams to kill cancer cells. It can be used before surgery to shrink tumors, after surgery to kill any remaining cancer cells, or as a palliative treatment to relieve symptoms.
How does chemotherapy play a role in esophageal cancer treatment?
Chemotherapy uses drugs to kill cancer cells throughout the body. It can be used before surgery to shrink tumors, after surgery to kill remaining cancer cells, or as a palliative treatment to alleviate symptoms.
What is targeted therapy and how is it used in the treatment of esophageal cancer?
Targeted therapy is a treatment approach that specifically targets cancer cells while minimizing damage to healthy cells. It may be used in combination with other treatments or as a standalone therapy for esophageal cancer, depending on the individual case.
How does immunotherapy help in the treatment of esophageal cancer?
Immunotherapy helps the body’s immune system recognize and attack cancer cells. It can be used in certain cases of esophageal cancer to enhance the body’s natural defenses against the disease.
What are clinical trials and how can they benefit esophageal cancer treatment?
Clinical trials are research studies that evaluate new or experimental treatments for esophageal cancer. They offer patients access to potentially breakthrough therapies and contribute to the advancement of cancer care.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.





