Welcome to our article on diverticulitis symptoms, where we will help you recognize the early signs of this condition. Diverticulitis is a condition characterized by the inflammation or infection of small pouches (diverticula) in the digestive tract. It is important to be aware of the symptoms so that you can seek medical attention promptly.
Table of Contents
ToggleRecognizing diverticulitis symptoms early is crucial for timely diagnosis and treatment. Common signs include constant abdominal pain, nausea, vomiting, fever, abdominal tenderness, and changes in bowel habits. If you experience unexplained abdominal pain along with a fever and constipation or diarrhea, it is important to consult a healthcare professional.
By understanding the early signs of diverticulitis, you can take proactive steps towards managing your health effectively. Stay tuned for more information on the causes, risk factors, and treatment options for diverticulitis.
What Is Diverticulitis and Diverticulosis?
Diverticulitis is a condition characterized by inflamed or infected diverticula, which are small pouches that can form in the lining of the colon. On the other hand, diverticulosis refers to the presence of these pouches without inflammation or infection. Diverticula are most commonly found in the lower part of the large intestine and are more common as people age.
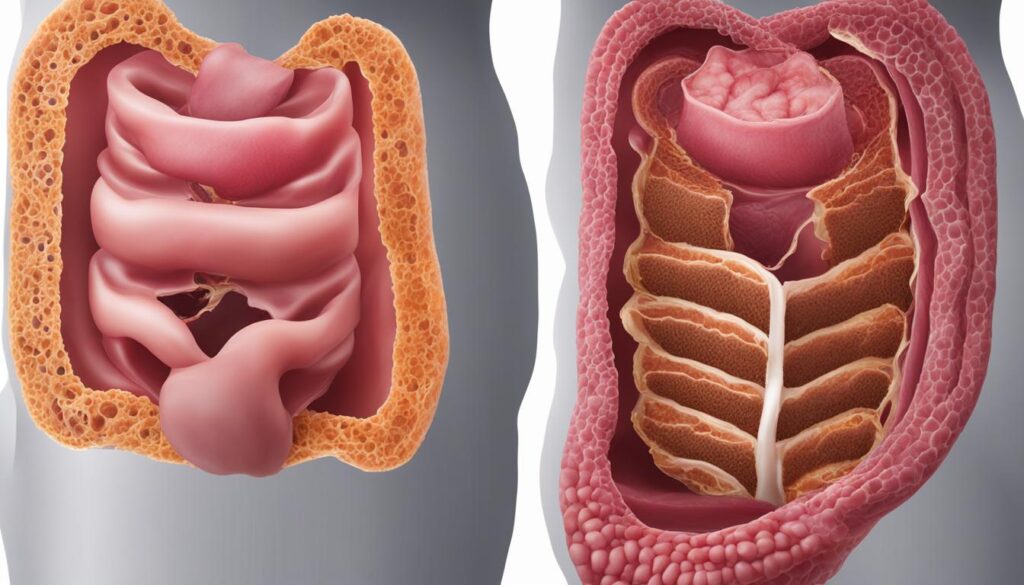
Diverticulosis and diverticulitis are conditions that affect the digestive tract. These conditions involve the presence of pouch-like structures called diverticula in the lining of the colon or large intestine. Diverticula are small, bulging pouches that can develop due to weak spots in the colon wall.
In the case of diverticulosis, these pouches are present but usually do not cause any symptoms or complications. However, when diverticula become inflamed or infected, it leads to diverticulitis. This can result in a range of symptoms and complications.
Diverticulitis occurs when these pouches become inflamed or infected. The exact cause of diverticular inflammation is not fully understood, but it is believed to be related to factors such as diet, lifestyle, and age. Diverticula are more common in older adults, and a low-fiber diet can increase the risk of diverticulitis.
The Connection Between Diverticulosis and Diverticulitis
Diverticulosis is often considered a precursor to diverticulitis. In diverticulosis, the presence of diverticula is not necessarily problematic, and most people with diverticulosis do not experience any symptoms. However, if the diverticula become inflamed or infected, it can lead to diverticulitis.
Some people may develop diverticulitis without having diverticulosis. In these cases, the diverticula may have formed in a short period of time due to factors such as inflammation or injury to the colon wall.
It is important for individuals with diverticulosis to take steps to prevent the development of diverticulitis. This can include adopting a high-fiber diet, managing stress, staying hydrated, and maintaining a healthy lifestyle with regular exercise.
| Diverticulosis | Diverticulitis |
|---|---|
| Presence of diverticula in the colon lining | Inflammation or infection of the diverticula |
| Usually asymptomatic | Can cause a range of symptoms and complications |
| Common in older adults | Can occur at any age |
| Can be managed with diet and lifestyle changes | May require medical intervention or surgery |
Common Symptoms of Diverticulitis
Recognizing the symptoms of diverticulitis is crucial for early detection and timely treatment. The condition manifests with various symptoms, including:
- Constant and severe abdominal pain, particularly on the lower left side. This pain may be persistent and worsen over time.
- Feelings of nausea and the urge to vomit, which can accompany the abdominal discomfort.
- Fever, often as a sign of an underlying infection in the inflamed diverticula.
- Abdominal tenderness, where the affected area may be sensitive to touch or pressure.
- Changes in bowel habits such as constipation or diarrhea, which can be alternating or persistent.
By paying attention to these symptoms, you can take the necessary steps to seek prompt medical attention and initiate appropriate treatment. Early intervention is essential for managing diverticulitis effectively and preventing potential complications.
Understanding Abdominal Pain in Diverticulitis
Abdominal pain is a primary symptom of diverticulitis and often the most prominent one. The pain tends to be constant and localized in the lower left side of the abdomen. However, the location and intensity of the pain may vary among individuals.
The severity of the pain can range from mild discomfort to acute and debilitating. It is important to note that the pain may worsen with movement, eating, or after bowel movements.
Although diverticulitis is commonly associated with left-sided abdominal pain, it is crucial to consult a healthcare professional for an accurate diagnosis, as other conditions may also present similar symptoms. A medical evaluation will help determine the underlying cause and provide appropriate treatment.

| Symptoms | Common Manifestations |
|---|---|
| Abdominal Pain | Constant, severe pain in the lower left side of the abdomen |
| Nausea and Vomiting | Feelings of queasiness and the urge to vomit |
| Fever | Rise in body temperature, indicating an underlying infection |
| Abdominal Tenderness | Sensitivity to touch or pressure in the affected area |
| Changes in Bowel Habits | Constipation or diarrhea, alternating or persistent |
Causes and Risk Factors of Diverticulitis
Diverticulitis is a condition that occurs when weak areas in the colon allow the development of small pouches called diverticula. These pouches can tear, leading to inflammation and infection. Understanding the Diverticulitis Causes and risk factors of diverticulitis can help you make informed choices about your health.
Weak Places in the Colon
The exact cause of weak areas in the colon is not fully understood. However, it is believed that pressure within the colon can push against the weak spots, causing diverticula to form. Over time, these weak areas may become more susceptible to tearing and infection.
Risk Factors
Several risk factors can increase the likelihood of developing diverticulitis:
- Aging: Diverticulitis becomes more common as people age.
- Obesity: Being overweight or obese can put additional strain on the colon.
- Smoking: Smoking weakens the walls of the colon, making it more prone to diverticula formation.
- Lack of exercise: Regular physical activity helps maintain a healthy colon function.
- Low-fiber diet: Consuming a diet low in fiber can contribute to constipation and increased pressure in the colon.
- Certain medications: Some medications, such as steroids and nonsteroidal anti-inflammatory drugs, may increase the risk of diverticulitis.
By understanding these causes and risk factors, you can take proactive steps to reduce your risk of developing diverticulitis. Making lifestyle changes, such as maintaining a healthy weight, quitting smoking, engaging in regular exercise, and adopting a high-fiber diet, can contribute to a healthier colon and minimize the chances of diverticula formation.
Complications and Prevention of Diverticulitis
Diverticulitis can lead to various complications that can significantly impact your health. It’s essential to be aware of these potential complications so you can take necessary preventive measures. Some of the complications associated with diverticulitis include:
- Development of an abscess: In some cases, the inflamed diverticula can lead to the formation of an abscess, which is a collection of pus. This can cause severe pain and may require drainage or surgical intervention.
- Blockage in the bowel: Severe inflammation or scarring due to repeated bouts of diverticulitis can cause a blockage in your bowel, leading to constipation, bloating, and discomfort.
- Formation of a fistula: Diverticulitis can sometimes result in the formation of an abnormal passageway, known as a fistula, between the colon and nearby organs, such as the bladder or vagina. This can cause infections and other complications.
- Peritonitis: In rare cases, untreated diverticulitis can lead to peritonitis, a serious condition characterized by inflammation of the lining of the abdominal cavity. Peritonitis is a medical emergency and requires immediate attention.
To reduce the risk of developing diverticulitis and its complications, certain preventive measures can be taken:
- Exercise regularly: Engaging in physical activities such as walking, jogging, or cycling can help maintain proper bowel function and reduce the risk of diverticulitis.
- Follow a high-fiber diet: Consuming foods rich in fiber, such as fruits, vegetables, whole grains, and legumes, can promote regular bowel movements and prevent the formation of diverticula.
- Stay hydrated: Drinking plenty of fluids, especially water, can help keep your stool soft and prevent constipation, which can contribute to diverticulitis.
- Avoid smoking: Smoking has been linked to an increased risk of diverticulitis. Quitting smoking or avoiding tobacco products altogether can significantly lower your chances of developing this condition.
- Maintain a healthy lifestyle: Adopting a healthy lifestyle, including managing stress, maintaining a healthy weight, and avoiding excessive alcohol consumption, can contribute to overall digestive health and reduce the risk of diverticulitis.
Foods High in Fiber
| Fiber-Rich Foods | Amount of Fiber per Serving (grams) |
|---|---|
| Almonds | 3.5 |
| Beans (kidney, black, pinto) | 6-8 |
| Broccoli (cooked) | 5 |
| Chickpeas | 8 |
| Raspberries | 8 |
| Pear | 5.5 |
| Sweet Potato (baked with skin) | 5 |
| Quinoa | 2.6 |
Adding these fiber-rich foods to your diet can promote bowel regularity and aid in the prevention of diverticulitis. Make sure to consult with a healthcare professional or dietitian for personalized dietary recommendations.
By taking preventive measures and making healthy lifestyle choices, you can reduce the risk of diverticulitis and its complications, enabling you to lead a healthier and more comfortable life.
Diagnosis and Treatment of Diverticulitis
If you experience symptoms of diverticulitis, it is crucial to seek medical attention for proper diagnosis and treatment. Diverticulitis diagnosis involves a thorough evaluation of your symptoms, medical history, and physical examination. Your doctor may also order additional tests, such as:
- CT scan: This imaging test can help visualize the inflamed diverticula and detect any complications, such as abscesses or perforations.
- Blood tests: These can help determine if you have an infection, assess your overall health status, and rule out other possible causes of your symptoms.
- Colonoscopy: In some cases, a colonoscopy may be recommended to rule out other conditions or to evaluate the extent of diverticulosis.
The treatment approach for diverticulitis depends on the severity of your symptoms. Mild cases can often be managed with:
- Rest: Giving your digestive system a break by avoiding solid foods and sticking to a liquid or low-fiber diet can help relieve symptoms and promote healing.
- Dietary changes: After the acute phase, gradually reintroducing high-fiber foods can help prevent future flare-ups and promote bowel regularity.
- Antibiotics: If your diverticulitis is accompanied by an infection, your doctor may prescribe antibiotics to help fight the infection.
However, severe or recurring cases of diverticulitis may require surgical intervention. Surgery may be recommended if you experience:
- Severe abdominal pain that does not respond to conservative measures.
- Complications such as abscesses, perforation, or fistulas.
- Recurrent attacks of diverticulitis despite medical management.
Conclusion
Early detection plays a crucial role in the management of diverticulitis. By being aware of the symptoms and seeking prompt medical attention, you can effectively manage the condition and reduce the risk of complications. It is important to remember that treatment options vary based on the severity of the condition.
In less severe cases, rest and dietary changes can be effective in relieving symptoms. However, for more severe or recurring cases, surgical intervention may be necessary. Consulting with a healthcare professional will help determine the most appropriate treatment plan for your specific situation.
Aside from medical interventions, incorporating lifestyle changes can also make a significant difference in preventing diverticulitis. Regular exercise can promote healthy digestion and bowel movements, while following a high-fiber diet can help maintain the health of your digestive system. By making these lifestyle changes, you can reduce the likelihood of developing diverticulitis and support your overall digestive health.
FAQ
What are the symptoms of diverticulitis?
Common symptoms of diverticulitis include constant abdominal pain, nausea, vomiting, fever, abdominal tenderness, and changes in bowel habits.
What is diverticulosis and diverticulitis?
Diverticulosis is the development of small pouches (diverticula) in the digestive tract, while diverticulitis refers to when these pouches become inflamed or infected.
What causes diverticulitis?
Diverticulitis is caused by weak areas in the colon that allow the development of diverticula. These pouches can tear, leading to inflammation and infection.
What are the risk factors for developing diverticulitis?
Several risk factors can increase the likelihood of developing diverticulitis, including aging, obesity, smoking, lack of exercise, a low-fiber diet, and certain medications such as steroids and nonsteroidal anti-inflammatory drugs.
What complications can arise from diverticulitis?
Complications of diverticulitis can include the development of an abscess, a blockage in the bowel, the formation of an abnormal passageway (fistula), or peritonitis, which is a medical emergency.
How can diverticulitis be prevented?
To prevent diverticulitis, it is important to exercise regularly, consume a high-fiber diet, drink plenty of fluids, avoid smoking, and maintain a healthy lifestyle.
How is diverticulitis diagnosed and treated?
If you experience symptoms of diverticulitis, it is crucial to seek medical attention for proper diagnosis and treatment. Mild cases of diverticulitis can be treated with rest, dietary changes, and antibiotics. However, severe or recurring cases may require surgery to manage the condition effectively.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.





