Chronic pancreatitis life expectancy varies widely depending on the cause, lifestyle factors, and how early treatment begins. Most people with well-managed chronic pancreatitis live into normal old age. Those who continue drinking alcohol, smoke heavily, or develop pancreatic cancer face significantly shorter survival.
Table of Contents
ToggleWhat Is Chronic Pancreatitis?
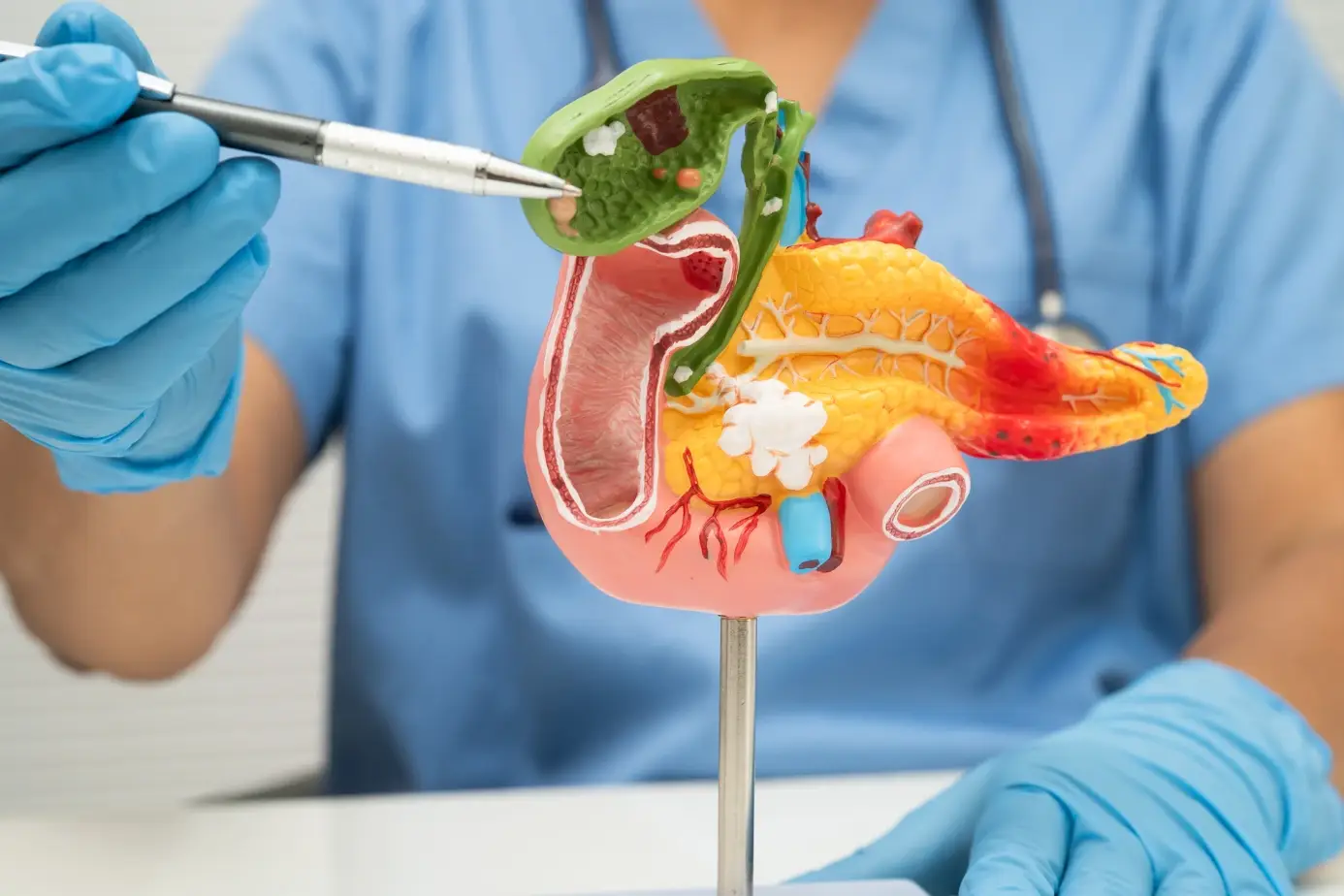
Chronic pancreatitis is long-term inflammation of the pancreas that causes permanent scarring over time. Unlike acute pancreatitis, which flares suddenly and often resolves, chronic pancreatitis is progressive. Each flare-up leaves more scar tissue. Over years, that scarring reduces the pancreas’s ability to produce digestive enzymes and insulin.
The result: patients develop malnutrition, chronic pain, and eventually diabetes. In some cases, the damaged tissue becomes cancerous. This progression is what makes chronic pancreatitis life expectancy a serious consideration, particularly when the condition goes unmanaged.
Chronic Pancreatitis Life Expectancy
A large study published in the journal Gut found that patients with chronic pancreatitis had a 20-year mortality rate of approximately 50%. However, that figure includes patients who continued alcohol use, developed cancer, and had late diagnoses.
Patients who stopped drinking, maintained nutrition, and received consistent medical care had outcomes much closer to the general population.
Key survival data:
- Around 70% of patients survive 10 years after diagnosis
- Around 45 to 50% survive 20 years
- Alcohol-related cases have a lower 20-year survival than non-alcohol-related cases
- Patients who stop drinking after diagnosis add an estimated 5 to 10 years to their survival compared to those who continue
Chronic pancreatitis life expectancy is a range, and lifestyle factors move a patient significantly within that range.
Factors That Affect Life Expectancy in Chronic Pancreatitis
Cause of the Disease
The causes of chronic pancreatitis shape the long-term outlook directly.
- Alcohol-related: Accounts for 70% of cases in Western countries. Continued alcohol use after diagnosis is the single strongest predictor of early death in chronic pancreatitis. Patients who stop drinking within the first year of diagnosis have measurably better survival.
- Genetic causes: Mutations in genes like PRSS1, SPINK1, and CFTR cause hereditary pancreatitis. These patients develop disease earlier, often in childhood or early adulthood, and carry a lifetime pancreatic cancer risk of 40% by age 70.
- Autoimmune pancreatitis: Responds well to steroid treatment. With proper management, this form has a better prognosis than alcohol-related disease.
- Idiopathic (unknown cause): Represents about 20% of cases. Prognosis varies and depends largely on how aggressively complications are managed.
Lifestyle Factors
- Continued alcohol use: Patients who keep drinking after diagnosis have double the mortality risk compared to those who stop. Alcohol directly damages pancreatic cells and accelerates scarring.
- Smoking: Smokers with chronic pancreatitis develop pancreatic cancer at twice the rate of non-smokers with the same condition. Smoking also accelerates calcification (hardening) of the pancreas, which worsens pain and digestion faster.
- Nutrition status: Malnutrition in chronic pancreatitis leads to muscle wasting, immune suppression, and poor wound healing. Patients with a body mass index below 18.5 have significantly worse outcomes than those who maintain adequate nutrition.
Severity and Disease Progression
- Frequent flare-ups cause cumulative damage. Each attack destroys more functional tissue.
- Patients with calcifications visible on CT scan have more advanced disease and a higher risk of complications.
- Loss of more than 90% of pancreatic function causes exocrine insufficiency, where the body cannot absorb fat or fat-soluble vitamins (A, D, E, K). This stage dramatically worsens nutritional status without enzyme replacement therapy.
Genetic Pancreatitis Life Expectancy
Hereditary pancreatitis, caused by PRSS1 gene mutations, starts earlier than alcohol-related disease. Symptoms typically appear between ages 5 and 15. By the time patients reach their 40s and 50s, they have lived with pancreatic inflammation for decades.
The cumulative cancer risk is the most significant factor in genetic pancreatitis life expectancy:
- Lifetime risk of pancreatic cancer in PRSS1 mutation carriers reaches 40% by age 70
- Smoking in this group pushes that risk even higher
- Regular surveillance with MRI or endoscopic ultrasound every 1 to 2 years is recommended from age 40 onwards for PRSS1 carriers
Patients with genetic pancreatitis who do not smoke and receive regular surveillance have better outcomes than those who go unmonitored. The cancer risk is the primary threat to survival in this group, not the pancreatitis itself.
Complications Affecting Survival in Pancreatitis
Complications affecting survival in pancreatitis are responsible for most of the excess mortality in this condition. The pancreatitis itself rarely kills directly. The downstream damage does.
Diabetes (type 3c diabetes): When scarring destroys insulin-producing beta cells, diabetes develops. Type 3c diabetes, the form caused by pancreatic disease, is harder to manage than type 2 diabetes. Poorly controlled diabetes in chronic pancreatitis accelerates kidney damage, nerve damage, and cardiovascular disease.
Malnutrition: Exocrine insufficiency reduces the body’s ability to absorb fat and fat-soluble vitamins. Without enzyme replacement, patients lose weight progressively despite eating. Vitamin D deficiency leads to bone fractures. Vitamin K deficiency impairs blood clotting.
Chronic pain: Persistent severe pain leads many patients to opioid dependence. Long-term opioid use carries its own mortality risk and reduces quality of life significantly.
Pancreatic cancer: The most serious complication. Chronic pancreatitis increases pancreatic cancer risk 13 to 16 times compared to the general population. Among complications affecting survival in pancreatitis, cancer carries the worst prognosis, with a 5-year survival rate of around 10 to 12% for pancreatic adenocarcinoma.
Treatment Impact on Chronic Pancreatitis Survival
The treatment impact on chronic pancreatitis survival is significant and measurable.
Pain management: Untreated pain leads to opioid dependency, poor nutrition, and reduced activity. Structured pain management, including nerve blocks (celiac plexus block) and endoscopic procedures to clear blocked ducts, reduces opioid use and improves quality of life. Patients with controlled pain maintain better nutrition and activity levels.
Pancreatic enzyme replacement therapy (PERT): Enzymes like pancrelipase (brand name Creon) replace the digestive enzymes the damaged pancreas cannot produce. PERT directly prevents malnutrition by restoring fat absorption. Patients on adequate PERT doses maintain weight and avoid vitamin deficiencies that otherwise accelerate decline.
Nutritional support: Some patients require enteral nutrition (feeding through a tube into the small intestine) during severe flare-ups when eating is not possible. Medium-chain triglyceride (MCT) supplements absorb without bile acids, making them useful for patients with severe fat malabsorption.
Endoscopic and surgical intervention: When the pancreatic duct is blocked by stones or strictures, endoscopic procedures (ERCP with stone removal) or surgery (Frey procedure, Whipple procedure) relieve pressure and reduce pain. Surgical drainage procedures shows that around 80% of patients report meaningful pain reduction post-surgery.
How Lifestyle Changes Influence Life Expectancy
The two changes with the strongest effect on survival are alcohol cessation and smoking cessation.
- Alcohol cessation: Patients who stop drinking within the first 12 months of diagnosis slow disease progression significantly. Pain episodes become less frequent. The rate of new scarring decreases. 5-year survival in abstinent patients is roughly 20 to 30% higher than in those who continue drinking.
- Smoking cessation: Stopping smoking reduces pancreatic cancer risk over time and slows calcification. Patients who stop smoking before significant calcification develops have better long-term duct function.
- Maintaining nutrition: Patients who work with a dietitian and use PERT consistently maintain weight and avoid the muscle wasting that shortens survival in this condition.
- Regular monitoring: Six-monthly or annual imaging catches complications, including pseudocysts, duct strictures, and early cancer, at a stage where treatment is still effective.
What Reduces Life Expectancy in Chronic Pancreatitis
Four factors consistently shorten chronic pancreatitis life expectancy across research studies:
- Continued alcohol use after diagnosis: The strongest single predictor of early death
- Late diagnosis: Patients diagnosed after cirrhosis, significant diabetes, or severe malnutrition has already developed start at a worse baseline
- Untreated exocrine insufficiency: Patients not on PERT who develop severe malnutrition lose lean muscle mass rapidly; this weakens immune function and cardiovascular health
- Unmonitored disease: Missing follow-up appointments means complications like pseudocysts, bile duct strictures, and early cancer go undetected until they are advanced
Living With Chronic Pancreatitis Long-Term
Living long-term with this condition is realistic for patients who manage it actively. Around 70% of patients survive a decade past diagnosis. Many of those live two decades or more.
The practical approach includes:
- Taking PERT with every meal and snack, not just large meals
- Attending imaging reviews every 12 months, or every 1 to 2 years for genetic pancreatitis patients after age 40
- Seeing a dietitian at least twice a year to adjust nutrition support as the disease changes
- Managing diabetes with an endocrinologist familiar with type 3c diabetes, since standard type 2 diabetes management protocols do not apply directly
- Treating pain through a structured program rather than self-managing with alcohol (which some patients unfortunately use as a pain coping mechanism, compounding the damage)
FAQs: Chronic Pancreatitis Life Expectancy
What is the life expectancy for chronic pancreatitis?
Around 70% of patients survive 10 years after diagnosis. 45 to 50% survive 20 years. Patients who stop drinking, control diabetes, and use enzyme replacement therapy have outcomes significantly closer to the general population than those who do not.
Can you live a long life with chronic pancreatitis?
Yes. Patients who stop alcohol, maintain nutrition with PERT, and attend regular follow-ups live well into old age. The condition shortens life primarily through complications like cancer and malnutrition, both of which are reduced through consistent management.
Does alcohol reduce survival in pancreatitis?
Yes, directly. Continued alcohol use after diagnosis doubles mortality risk in chronic pancreatitis. Patients who stop drinking within 12 months of diagnosis slow disease progression measurably and add an estimated 5 to 10 years compared to those who keep drinking.
Is chronic pancreatitis life-threatening?
Yes, long-term. The 20-year mortality rate is approximately 50%, higher than many cancers. Death typically results from pancreatic cancer, diabetes complications, or malnutrition rather than acute pancreatitis itself. Early diagnosis and lifestyle changes reduce this risk substantially.
Does treatment improve life expectancy?
Yes. PERT prevents malnutrition-related death. Surgical drainage procedures reduce pain and slow duct damage. Celiac plexus blocks reduce opioid dependency. Each intervention targets a specific pathway that, if left untreated, shortens life expectancy.
What complications affect survival?
Pancreatic cancer (13 to 16 times higher risk than the general population), type 3c diabetes with its unstable blood sugar control, severe malnutrition from exocrine insufficiency, and opioid dependency from unmanaged pain are the four complications most directly linked to shortened survival.
Is genetic pancreatitis more serious?
Yes, in one specific way. PRSS1 gene mutation carriers have a 40% lifetime risk of pancreatic cancer by age 70, compared to 13 to 16% in alcohol-related disease. Earlier disease onset means more years of cumulative damage. Surveillance MRI from age 40 onwards is essential for this group.
Can lifestyle changes improve survival?
Yes. Stopping alcohol and smoking are the two changes with the strongest evidence. Abstaining from alcohol after diagnosis improves 5-year survival by 20 to 30%. Stopping smoking reduces pancreatic cancer risk over time. Both changes together give the best chance of a normal lifespan with chronic pancreatitis.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.