Yes, you can live without a gallbladder. Completely. More than 700,000 Americans get their gallbladder removed every year, and most return to normal life within weeks. The body adjusts, digestion continues, and for most people, life after surgery is not noticeably different from before.
Table of Contents
ToggleThe gallbladder is useful, but not essential. When it causes problems, such as gallstones or chronic inflammation, removing it is safer than keeping it. The liver still produces bile, and digestion still works. The adjustment period is real, but it is temporary for most people.
What Does the Gallbladder Do?
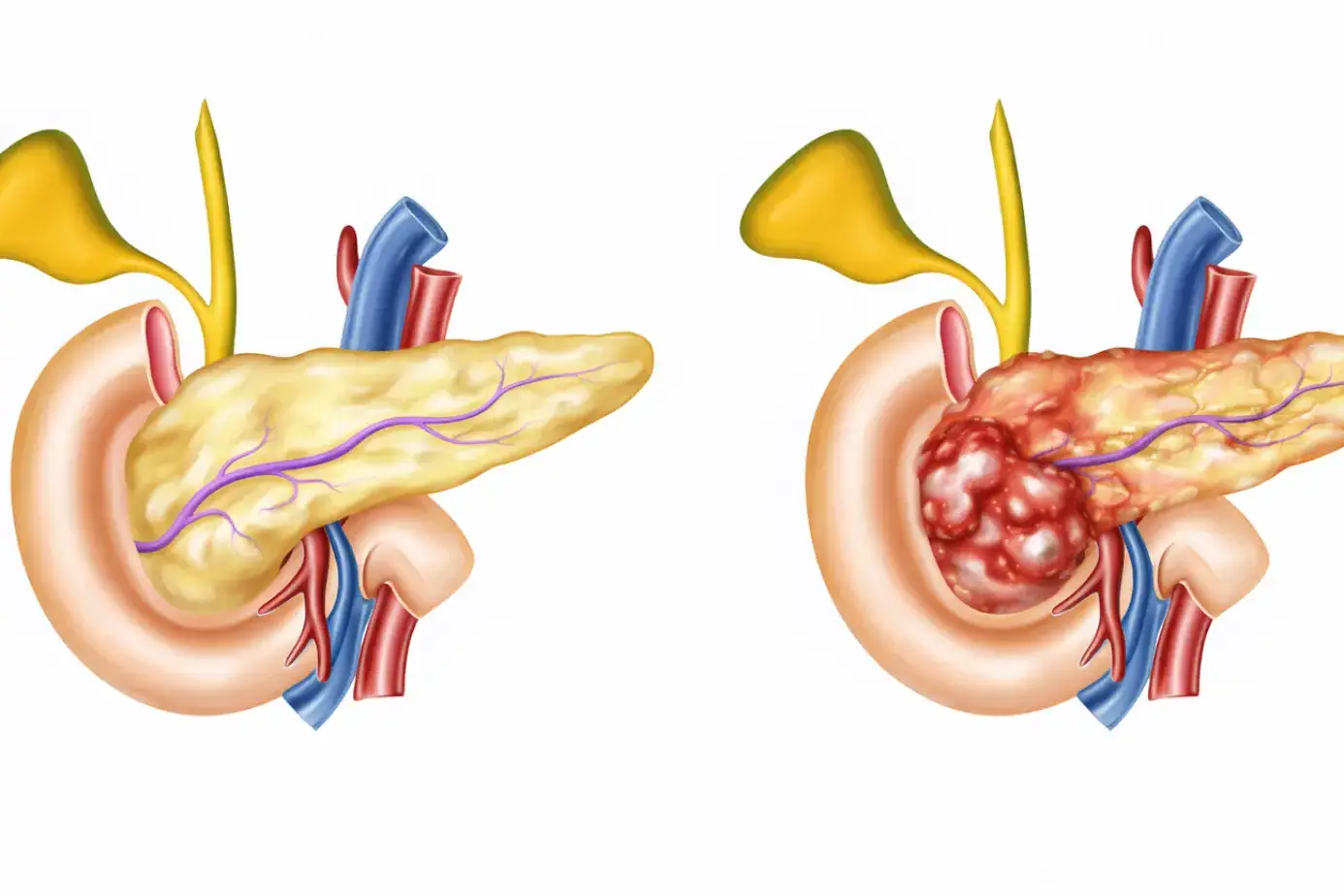
The gallbladder sits under the liver and stores bile, a digestive fluid the liver makes constantly. When you eat a fatty meal, the gallbladder squeezes and releases bile into the small intestine to help break down fats.
Without the gallbladder, bile does not get stored or concentrated. It drips continuously from the liver into the intestine instead, regardless of whether food is present.
What Happens After Gallbladder Removal?
What happens after gallbladder removal is a shift in how bile moves through your digestive system. Instead of releasing bile in controlled bursts during meals, the liver trickles a steady, diluted stream of bile into the small intestine around the clock.
The key changes:
- Bile is less concentrated than it was when stored in the gallbladder
- Bile enters the intestine even when no food is present
- Fat digestion becomes slightly less efficient, especially with large or greasy meals
- The colon receives more bile acids than it did before surgery
These changes are noticeable for the first few weeks and then settle down. The gut adjusts. Some people experience ongoing mild symptoms. A smaller group has persistent issues that need medical attention.
How the Body Adapts Without a Gallbladder
The liver does not slow down bile production after the gallbladder is removed. It keeps making bile at the same rate. What changes is delivery. The bile duct, which connected the gallbladder to the intestine, gradually expands slightly over months to hold a small reserve of bile. This is not the same as a gallbladder, but it softens the shift.
The small intestine also adapts. Over weeks to months, the intestinal cells become better at handling the constant low-level bile flow. Symptoms like bloating and diarrhea, which are common in the first month after surgery, often reduce significantly by the three to six month mark.
The body adapting without a gallbladder follows a general timeline:
- Weeks 1 to 4: Most significant adjustment period. Diarrhea, bloating, and discomfort are common.
- Months 1 to 3: Symptoms typically reduce as the intestine adapts to continuous bile flow.
- Months 3 to 6: Most people reach a new digestive baseline with minimal ongoing symptoms.
- Beyond 6 months: Around 10 to 15% of patients still have chronic diarrhea or discomfort at this stage.
Common Symptoms After Gallbladder Removal
Bloating and Gas Without Gallbladder
Bloating and gas without gallbladder are among the most reported post-surgery complaints. The cause is the continuous drip of bile into the intestine. When bile is present without food to digest, gut bacteria ferment the bile acids. This produces gas.
Fatty meals make it worse. The intestine, now working with diluted bile, struggles to fully break down fat, especially in large amounts. Undigested fat feeds bacteria in the colon, which adds more gas and bloating.
Bloating and gas without gallbladder tend to peak in the first month and improve as the gut adjusts to the new bile flow pattern.
Diarrhea and Loose Stools
Diarrhea after gallbladder removal is common. Around 20% of patients experience it in the first few weeks. Bile that reaches the colon draws water in, speeding up bowel transit. More bile reaches the colon than before because the gallbladder is no longer storing and releasing it in controlled amounts.
For most people, this settles within one to two months. For some, it persists longer and needs treatment.
Bile Acid Malabsorption After Cholecystectomy
Bile acids are supposed to be reabsorbed in the last section of the small intestine and recycled back to the liver. After gallbladder removal, the constant bile flow overwhelms this recycling system. Excess bile acids spill into the colon. Bile acids in the colon irritate the lining, pull in water, and trigger diarrhea.
Bile acid malabsorption after cholecystectomy affects roughly 10% of patients who have chronic diarrhea after surgery. It does not resolve on its own. Treatment involves bile acid sequestrants like cholestyramine or colesevelam, which bind the excess bile acids in the colon and stop the irritation.
A SeHCAT scan (a nuclear medicine test measuring bile acid retention) is the standard diagnostic tool for this condition. Most GPs do not order it automatically. If diarrhea persists beyond three months post-surgery, pushing for this test is reasonable.
Foods to Avoid Without Gallbladder
Foods to avoid without gallbladder are primarily high-fat and heavily processed options, at least during the adjustment period.
Large portions of fat overwhelm the diluted bile supply and cause cramping, bloating, and diarrhea.
Foods to avoid without gallbladder in the first three months:
- Fried foods: chips, fried chicken, french fries
- Full-fat dairy: butter, cream, full-fat cheese, whole milk
- Fatty cuts of meat: bacon, sausages, lamb chops
- Heavy sauces: cream-based pasta sauces, gravies, salad dressings with oil
- Large portions in a single sitting, regardless of fat content
- Spicy foods, which can irritate an already-adjusting digestive system
After the three to six-month mark, you can reintroduce these foods gradually without consistent problems.
Long-Term Effects of Living Without a Gallbladder
You can live without a gallbladder long-term without significant problems.
Studies tracking patients 5 to 10 years after cholecystectomy (the medical term for gallbladder removal) show that around 85% report no ongoing digestive symptoms. The remaining 15% have varying degrees of persistent diarrhea, bloating, or fat intolerance.
Gallbladder removal may increase the risk of non-alcoholic fatty liver disease and metabolic syndrome in patients who were already overweight. The connection is not fully understood, but the constant bile flow changes how fats and bile acids are processed by the liver over time.
Does Gallbladder Removal Affect Life Expectancy?
You can live without a gallbladder with a normal lifespan. Gallbladder removal does not shorten life expectancy.
The surgery itself carries the standard surgical risks: infection, bleeding, bile duct injury. Bile duct injury during laparoscopic surgery occurs in roughly 0.3 to 0.5% of cases and requires further treatment when it happens. Beyond the surgical period, the operation has no effect on how long a person lives.
When Symptoms After Gallbladder Removal Are Not Normal
Most post-surgery symptoms are predictable and temporary. These are the signs that something needs medical evaluation:
- Diarrhea lasting more than three months without improvement
- Severe abdominal pain in the upper right area, which can indicate bile duct issues or retained stones
- Jaundice (yellowing of the skin or eyes), which signals a bile duct blockage
- Fever with abdominal pain, which suggests infection
- Unexplained weight loss, which requires investigation
- Recurrence of the exact pain that existed before surgery, which might mean a retained gallstone in the bile duct
Post-cholecystectomy syndrome is the clinical term for persistent symptoms after surgery that do not resolve. It affects roughly 10 to 15% of patients.
Causes include bile acid malabsorption, retained stones, sphincter of Oddi dysfunction, or an unrelated digestive condition that was mistakenly attributed to the gallbladder originally.
FAQs: Can You Live Without a Gallbladder?
Can you live normally without a gallbladder?
Yes. Around 85% of people who have their gallbladder removed report no ongoing digestive symptoms after six months. The liver continues producing bile, and the intestine adjusts to handle continuous bile flow. Normal diet, activity, and life expectancy are fully maintained for most patients.
What changes after gallbladder removal?
Bile flows continuously from the liver into the intestine instead of being stored and released with meals. This makes fat digestion slightly less efficient, especially with large or greasy meals. Diarrhea and bloating are common in the first month but typically resolve by month three.
Do you need a special diet forever?
No. High-fat food restrictions apply mainly to the first three to six months post-surgery. After the gut adapts, most people return to their normal diet. A small group with persistent bile acid malabsorption benefits from a lower-fat diet long-term, but that is not the typical outcome.
Is diarrhea common after surgery?
Yes. Around 20% of patients experience diarrhea in the first weeks post-surgery. It results from excess bile acids reaching the colon. For most patients, it resolves by month two. If it persists beyond three months, bile acid malabsorption is the likely cause and needs testing.
Can digestion return to normal?
Yes, for approximately 85% of patients. The adjustment period runs three to six months. After that, digestive function stabilizes. The bile duct expands slightly to hold a small reserve, and the intestinal lining adapts to handle the continuous bile flow more efficiently.
Does gallbladder removal affect lifespan?
No. Gallbladder removal does not affect life expectancy. The organ is non-essential. Lifespan outcomes depend on the underlying condition that required surgery, not the removal itself.
What is bile acid malabsorption?
Bile acid malabsorption after cholecystectomy occurs when excess bile acids bypass reabsorption in the small intestine and enter the colon, causing chronic diarrhea. It affects roughly 10% of post-surgery patients. A SeHCAT scan diagnoses it. Cholestyramine or colesevelam treats it effectively.
Should I avoid fatty foods completely?
No. Avoid high-fat meals for the first three to six months while the gut adjusts. After that, reintroduce them gradually. The key is portion size, not permanent elimination. Smaller meals with moderate fat are handled well once adaptation is complete.
About The Author

Medically reviewed by Dr. Nivedita Pandey, MD, DM (Gastroenterology)
Dr. Nivedita Pandey is a U.S.-trained gastroenterologist and hepatologist with extensive experience in diagnosing and treating liver diseases and gastrointestinal disorders. She specializes in liver enzyme abnormalities, fatty liver disease, hepatitis, cirrhosis, and digestive health.
All content is reviewed for medical accuracy and aligned with current clinical guidelines.